Objectives
Upon finishing this module, the student will be able to:
- Describe the different types of skull fracture
- Describe the different types of intracranial hemorrhage
- List the signs and symptoms of concussion
- Determine which children are low risk for clinically significant traumatic brain injury and can be discharged without imaging
- Initiate treatment for children with head injuries in the emergency department
Introduction
Head injury includes any injury to the scalp, skull, or brain. It is the most common type of injury requiring medical evaluation in children. While most injuries are mild, brain injury is the leading cause of death and disability in pediatric trauma patients.
Initial Actions and Primary Survey
Initial actions will depend on the presentation of the child. Some patients will present many hours after the initial trauma and be ambulatory on arrival. Others may present unconscious from the scene of the injury. If there is any concern of possible cervical spine injury or if the patient has altered mental status limiting exam, the spine should be immobilized immediately and a cervical collar placed. A complete primary and secondary survey should be completed to ensure the patient is stable and to assess for any other injuries.
Assigning the child a Glasgow Coma Scale score should be performed as part of the initial evaluation. Scoring for children and adults is the same, but infants and preverbal children must be assessed differently.
| Activity | Score | Child/ Adult | Score | Infant |
| Eye Opening | 4
3 2 1 | Spontaneous
To speech To pain None | 4
3 2 1 | Spontaneous
To speech/ sound To pain None |
| Verbal | 5
4 3 2 1 | Oriented
Confused Inappropriate Incomprehensible None | 5
4 3 2 1 | Coos/ babbles
Irritable cry Cries to pain Moans to pain None |
| Motor | 6
5 4 3 2 1 | Follows commands
Localizes to pain Withdraws to pain Abnormal flexion Abnormal extension None | 6
5 4 3 2 1 | Spontaneous movements
Withdraws to touch Withdraws to pain Abnormal flexion Abnormal extension None |
Presentation
There is a wide spectrum of presentation for children with head injuries. Some children will have only scalp hematomas, while others will suffer severe intracranial injuries and present with coma or seizures. Important injuries to consider in children with head trauma include skull fractures, intracranial hemorrhages, and concussion.
Skull fractures
Skull fractures are more common in infants than in older children, with the parietal bone being the bone most commonly fractured, and the frontal bone being the least commonly fractured. There are three categories of skull fractures:
- Linear skull fractures may have an overlying hematoma, but bony abnormalities are rarely palpated.
- Depressed skull fractures may be palpable on exam, with a depression or step-off felt when the skull is palpated.
- Basilar skull fractures are fractures to the base of the skull, and can include the temporal bone, occipital bone, sphenoid bone, or ethmoid bone. Although rare, these fractures require additional evaluation as they can result in tears in the meninges leading to leakage of cerebral spinal fluid. Patients with basilar skull fractures may have physical exam findings including raccoon eyes (periorbital ecchymosis in the absence of a direct blow to the face), Battle’s sign (ecchymosis over the mastoid process), hemotympanum, or drainage of cerebral spinal fluid from the nose.
Intracranial hemorrhage
Children with intracranial hemorrhage may present with a variety of symptoms, including headaches, frequent vomiting and altered mental status. Intracranial hemorrhage should be suspected in any patient presenting to the emergency department with decreased level of consciousness. There are four types of intracranial hemorrhage:
- Epidural hematomas occur when there is bleeding into the space between the skull and the dura mater. CT scan will show a convex, lens-shaped collection of blood. Blood generally does not cross suture lines. Many of these hemorrhages are caused by laceration of the middle meningeal artery, although venous bleeds can also occur. The classic presentation is a brief loss of consciousness with the trauma, followed by a lucid period and then deterioration. As epidural hematomas can accumulate rapidly, patients may change quickly and a timely diagnosis and neurosurgical intervention are key.
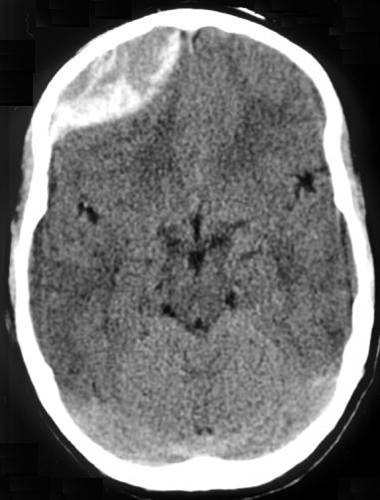
- Subdural hematomas occur when there is bleeding into the space between the dura and arachnoid membranes. They appear as concave or crescent-shaped collections of blood on CT scan, and can cross suture lines. These are generally caused by tears to the bridging veins between the cortex and venous sinuses. The hemorrhage occurs more slowly than in epidural hematomas, although still over a period of a few hours.
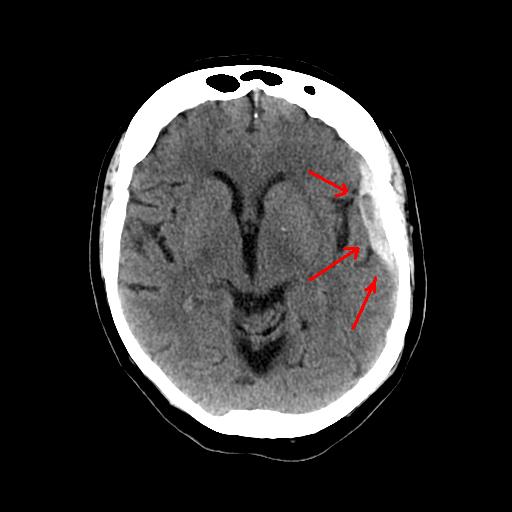
- Subarachnoid hemorrhages occur when there is bleeding into the space between the arachnoid membrane and the pia mater that surrounds the brain.
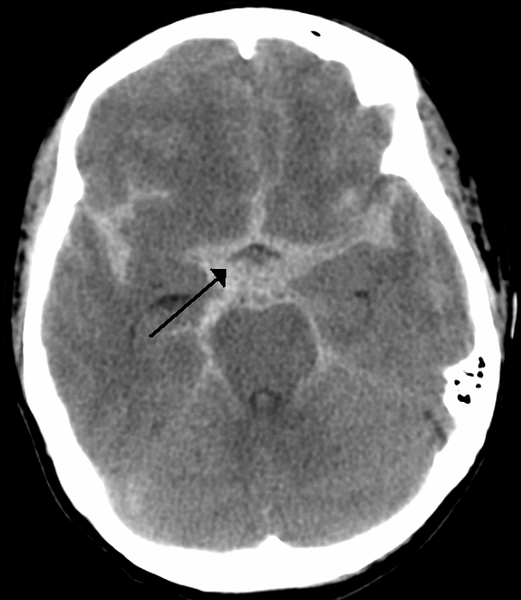
- Intraparenchymal hemorrhages occur when there is tearing of intraparenchymal blood vessels. Depending on the size, these can also cause mass effect and midline shift, and may be more difficult to manage surgically than extra-axial hemorrhages.
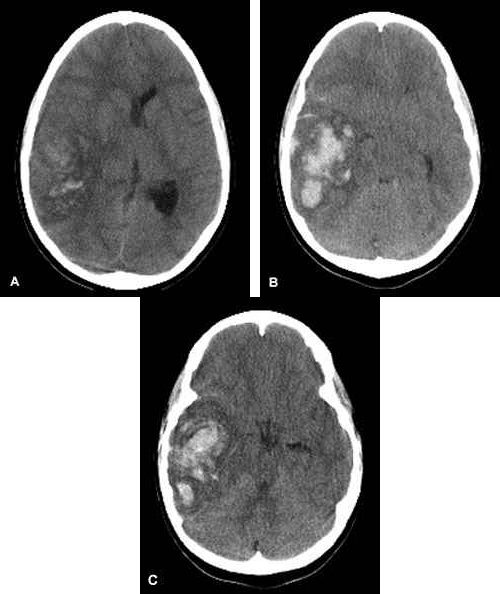
- When evaluating a CT scan with an intracranial hemorrhage, it is important to not only identify the type of hemorrhage, but also to note the size and whether the lesion is causing mass effect or midline shift.
Concussion
Concussion has been defined as a disturbance in brain function caused by a direct or indirect force to the head. Patients with concussion may present with a variety of symptoms, but imaging is unremarkable on these patients. A concussion should be suspected in a patient with recent head trauma who complains of headache, vomiting, unsteadiness, confusion, or other abnormal behaviors. Several tools exist to help team trainers and physicians evaluate patients with concussions, including the Sport Concussion Assessment Tool 2, or SCAT2.
Diagnostic Testing
One of the most difficult decisions when a child presents with a head injury is whether or not the child requires a CT scan to evaluate for fracture or intracranial injury. If the child presents with an abnormal neurologic exam or decreased level of consciousness, the decision is usually straightforward and imaging is ordered immediately. However, many children present after a head injury with complaints such as loss of consciousness, brief period of appearing “dazed”, vomiting, or scalp hematoma, but are alert and active on exam. It is more difficult determining which of these children require imaging.
In 2009, the Pediatric Emergency Care Applied Research Network (PECARN) published an article that has been used to help practitioners identify children at very low risk of clinically significant brain injuries following head trauma. The study evaluated 42,412 children under the age of 18 and GCS of 14-15 presenting to the ED for evaluation of head trauma. This study includes suggested algorithms to be used to identify those children who meet low risk criteria for a clinically significant brain trauma and can therefore be discharged without a CT scan. The criteria are different for children under 2 years, and for those 2 years or older.
Low risk criteria for children less than 2 years of age include an absence of any of the following:
- GCS 14 or less or other signs of altered mental status
- Palpable skull fracture
- Occipital, parietal, or temporal scalp hematoma
- History of loss of consciousness ≥5 seconds
- Severe mechanism of injury
- Not acting normally per the parent
Low risk criteria for children 2 years of age or older include absence of any of the following:
- GCS 14 or less or other signs of altered mental status
- Signs of basilar skull fracture
- History of loss of consciousness
- History of vomiting
- Severe mechanism of injury
- Severe headache
If children meet NONE of these criteria, they have a very low risk of clinically important traumatic brain injury, and can be discharged without CT. If children do have low GCS, altered mental status, or signs of skull fracture, CT head is recommended. For children who have GCS of 15, normal mental status, and no signs of skull fracture, but do have another risk factor, a period of observation vs CT scan may be considered.
Once a decision has been made to observe rather than obtain a CT scan, the question is always, “How long do I need to watch the patient?” A large study of children with mild head injuries found that the vast majority of children with intracranial hemorrhages will have worsening symptoms within 6 hours of the trauma. If children still appear well after a six hour observation period, they may be discharged home with instructions to return if the child is showing worsening symptoms.
Treatment
Treatment depends on the severity of the injury. It is important to ensure that all children with head injuries have adequate blood pressures and oxygen saturations as hypoxia and hypoperfusion of the brain may cause additional damage following a head injury. The head of the bed should be elevated to 30 degrees if there are any signs of increased intracranial pressure.
Linear skull fractures with no underlying hemorrhage will generally heal well and do not require admission if the child is otherwise well. Children with depressed skull fractures or basilar skull fractures should be evaluated by a neurosurgeon. Physicians should always keep the possibility of child abuse/maltreatment in mind when evaluating a child who sustains a skull fracture.
Intracranial hemorrhages should be evaluated by a neurosurgeon to determine if surgical intervention is indicated. Patients with small hemorrhages are often admitted for observation and supportive care, while those with large hemorrhages may go immediately to the operating room for drainage. For those with elevated intracranial pressure (ICP), hypertonic saline or mannitol may be used in an attempt to lower ICP. It is important to ensure that the patient has been volume resuscitated prior to use of mannitol in particular as it will cause diuresis. If there are signs of impending herniation, hyperventilation can be used temporarily while other treatment options are evaluated.
For more mild head injuries, supportive care with ondansetron for vomiting and acetaminophen or ibuprofen for headaches may be adequate. Children with concussions who participate in sports should not return to play until they are symptom free, and when they do return to play, they should gradually progress from light exercise to full contact sport participation rather than immediately returning to full play. All children with concussions should be cleared by either a physician or a qualified team trainer prior to returning to sports, and it is important to communicate this to families before they leave the emergency department.
Pearls and Pitfalls
- The classic presentation for epidural hematomas is loss of consciousness followed by a lucid period and then deterioration, while the presentation for subdural hematomas is generally gradual worsening of mental status over time
- Patients with isolated linear skull fractures can often be discharged, while those with depressed or basilar skull fractures require evaluation by a neurosurgeon
- Children who meet certain criteria have a very low risk of clinically significant brain injury, and can be discharged without imaging
- Children with concussion should not return to play until symptom-free, and should follow a gradual progression to full activity
References
- World Health Organization & UNICEF. World Report on Child Injury Prevention. 2010. Accessed at: http://whqlibdoc.who.int/publications/2008/9789241563574_eng.pdf?ua=1
- Wing R & James C. Pediatric head injury and concussion. Emergency Medicine Clinics of North America. 2013; 31 (3): 653-675.
- Sport Concussion Assessment Tool 2. Accessed at: http://www.cces.ca/files/pdfs/SCAT2%5B1%5D.pdf.
- Kupperman N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: A prospective cohort study. Lancet. 2009; 374: 1160-70.
- Hamilton M, Mrazik M, & Johnson DW. Incidence of delayed intracranial hemorrhage in children after uncomplicated minor head injuries. Pediatrics. 2010; 126: e33-39.
Image credits
Images are all state they can be shared with proper attribution. Site for images included here.
Epidural hematoma CT: “Epidural Hematoma”. Via Wikipedia
http://commons.wikimedia.org/wiki/File:Traumatic_acute_epidual_hematoma.jpg
Subdural hematoma CT: “Subdural Hematoma”. Via Wikipedia
http://en.wikipedia.org/wiki/Subdural_hematoma#mediaviewer/File:SDH.jpg
Subarachnoid hemorrhage CT: “Subarachnoid hemorrhage”. Via Wikipedia
http://commons.wikimedia.org/wiki/File:SubarachnoidP.png
Intraparenchymal hemorrhage CT: “Intraparenchymal hemorrhage”. Via Wikipedia
http://commons.wikimedia.org/wiki/File:Multiple_intraparenchymal_hemorrhage.jpg
