Biliary Disease
John Bouldin, MD, University of Arkansas for Medical Sciences, Christopher Fowler, DO, University of Arkansas for Medical Sciences
Editor: Amy Kule, MD, Loyola University Medical Center,
Last Updated: May 2019
Case Study
A 45-year old male presents to the ED with 3 days of right upper quadrant pain. He reports the pain is sharp, worsening, and radiates to his back. It is associated with multiple episodes of nausea and vomiting, as well as chills and sweats at home. He notes the pain is worse when he eats and admits that he has had pain like this multiple times over the past several years, but it normally improves over a couple of hours and has never been this severe. He reports that his daughter, who is visiting from out of town, told him that his skin appeared yellow. Vital signs in triage were T 39°C (102.2°F), HR 110 beats/minute, BP 110/75 mmHg, RR 22 breaths/minute, SpO2 98% on room air.
On exam, you immediately notice his skin and sclera have a yellow tint and he appears uncomfortable. He has tenderness to palpation over his right upper quadrant and is diaphoretic. Murphy sign is negative. The rest of his exam is unremarkable.
Objectives
Upon finishing this module, the student will be able to:
- Describe the spectrum of biliary tract diseases.
- Describe the classic history and physical exam findings for biliary tract disease.
- Delineate the differences among various biliary tract diseases
- List the typical laboratory findings for different biliary tract diseases.
- Discuss the advantages and limitations of the different radiologic studies utilized in the diagnosis and differentiation of biliary tract disease.
- Discuss the appropriate treatment and disposition decisions for patients with diseases of the biliary tract.
Introduction
Abdominal pain is the most common chief complaint for patients nationwide when presenting to the Emergency Department. Diseases of the biliary tract (gallbladder and bile ducts) are common and result in significant morbidity and mortality. In the United States 20% of all people will suffer from symptomatic gallstones (cholelithiasis) at some time in their lives. If untreated, 20-30% of these patients will develop serious complications of gallstones such as choledocholithiasis, cholecystitis, and cholangitis. Pancreatitis is also a common complication of gallstones but is outside the scope of this module.
Initial Actions and Primary Survey
As with all patients presenting to the Emergency Department, assessing their airway, breathing, and circulation is your first priority. Patients presenting with biliary pathology can have a wide range of severity—from relatively benign symptoms with temporary or intermittent discomfort to life-threatening presentations in septic shock. A full set of vitals, placing the patient on a cardiac monitor, and obtaining IV access are crucial initial actions. Once these are completed, a focused history and physical exam should be completed.
Presentation
The classic history finding in biliary pathology is biliary colic, which is also termed symptomatic cholelithiasis. This describes episodic right upper quadrant or epigastric pain associated with nausea and vomiting, which is caused by gallstones intermittently obstructing at the neck of the gallbladder. The pain may radiate to the back, right flank, tip of the right scapula, or right shoulder. Patients will often report previous episodes in association with eating fatty meals. In uncomplicated symptomatic cholelithiasis, this pain may last 4-6 hours before spontaneously resolving.
Pain lasting over 6 hours or with other associated features, such as fever, jaundice, or confusion suggest more serious causes and should prompt further evaluation for complications such as choledocholithiasis, cholecystitis, and cholangitis.
Symptomatic Cholelithiasis
Cholelithiasis (gallstones) occurs as a result of supersaturation of bile with cholesterol (70%), pigments such as bilirubin (20%), or both (10%) combined with delayed emptying of the gallbladder (stasis). Patients can have gallstones for years and remain asymptomatic. However, having a history of cholelithiasis puts patients at risk of complications described in this module.
Patients with symptomatic cholelithiasis experience biliary colic due to intermittent obstruction of the gallbladder neck by gallstones. Fatty meals exacerbate these painful episodes secondary to secretion of hormones that cause gallbladder contraction and bile release into the digestive tract to aid in the breakdown fats in the intestines. As noted above, these episodes typically last <6 hours and resolve spontaneously.
Choledocholithiasis
In cholelithiasis, gallstones remain in the gallbladder. In choledocholithiasis, the stone has moved out of the gallbladder and is obstructing the common bile duct. Once in the common bile duct, the stone obstructs flow from the contributing ducts—the cystic duct and the hepatic ducts. Since these stones often become lodged in the common bile duct, the pain they cause frequently lasts >6 hours.
With significant bile duct obstruction, there is a congestion of the biliary tree which causes a backflow of bile into the liver and eventually into the blood, leading to bilirubinemia. As the obstructions persists this can manifest systemically as jaundice. Typically the first place that jaundice is manifest is in the scleara of the eyes. Typical levels of bilirubin are >3 mg/dL However, patients with choledocholithiasis may not present with jaundice if the stone fails to cause complete or near-complete obstruction, allowing enough bilirubin to pass from the biliary system.
A high index of suspicion for choledocholithiasis must be kept in patients with biliary colic >6 hours since obstructing stones in the common bile duct place patients at increased risk of inflammatory and infectious complications such as cholecystitis and cholangitis. Patients presenting with biliary colic and jaundice should undergo choledocholithiasis workup in all cases.
Cholecystitis
Acute cholecystitis is inflammation of the gallbladder and is related to the presence of gallstones in 90-95% of cases. Acalculous cholecystitis occurs in <10% of cases and is seen more often in patients who are elderly, post-operative, or critically ill from other causes.
In calculous cholecystitis, the cystic duct is blocked by a gallstone, causing obstruction, pain, and, ultimately, inflammation. If untreated, this inflammation can progress to necrosis, gangrene, and perforation.
The primary history differences between cholecystitis and cholelithiasis include biliary colic >6 hours and constitutional symptoms such as fever and malaise.
On physical exam, patients can exhibit right upper quadrant and epigastric pain as seen in symptomatic cholelithiasis. A classic feature of cholecystitis is the presence of the Murphy sign. The Murphy sign is not simply pain in the right upper quadrant with palpation. The Murphy sign can be elicited by having the patient exhale fully, placing your hand at the midclavicular line of the right costal margin, and having the patient inhale. The test is positive if the patient stops inhalation and winces upon contact of the gallbladder with your hand. The sign must be absent when performed on the left for the test to be positive. However, it is worth noting that research has been highly variable on the usefulness of this sign in predicting presence of cholecystitis, with at least one large, recent study failing to find statistical significance in its use.
Patients with cholecystitis can have jaundice despite the stones typically obstructing the cystic duct. In some cases, the patient may have cholecystitis with choledocholithiasis. However, even without choledocholithiasis, jaundice and bilirubinemia can occur due to local liver inflammation from reaction to the adjacent inflamed gallbladder.
Despite presence of fever as a key feature of the diagnosis, roughly half of patients with acute cholecystitis do not have infected bile when cultured. The inflammation seen in cholecystitis is believed to be due to inflammatory marker release due to endothelium damage from obstruction and direct trauma from stones—though concomitant infection likely contributes to this inflammation in many patients.
Cholangitis
Cholangitis is inflammation of the bile ducts and is most often caused by a polymicrobial bacterial infection. Biliary obstruction – such as from a stone or neoplasm – serves as a major factor in its pathogenesis.
Features in ascending cholangitis are described by two classic combinations of findings:
Charcot Triad
- Fever
- Right upper quadrant pain
- Jaundice
Reynold Pentad—severe cases
- Fever
- Right upper quadrant pain
- Jaundice
- Confusion
Hypotension
Cholangitis is less common than cholecystitis but has significantly higher mortality if undiagnosed and untreated. Pain and jaundice are caused through similar mechanisms as seen in choledocholithiasis. Introduction of bacterial infection (typically of bowel flora) into this obstructive environment leads to the clinical presentations shown above. Unlike in cholecystitis, >90% of cultures in cholangitis will be positive. These cultures can be positive due to a wide array of pathogens. E. coli, Klebsiella, and Enterobacter account for most gram-negative cultures. Enterococcus accounts for many gram-positive cultures. Anaerobes, such as Bacteroides and Clostridia, are often present in mixed flora isolates. Patients presenting with the Reynold Pentad and signs of severe sepsis with possible septic shock require higher levels of care.
Diagnostic Testing
Laboratory evaluation of patients with suspected biliary pathology is routine. A complete blood count and liver function tests should be sent. A lipase should also be sent any time gallstone pathology is suspected due to high rates of concomitance with gallstone pancreatitis.
Lab findings are particularly helpful for differentiating cholelithiasis from choledocholithiasis and cholangitis. Lab findings are not as useful for differentiating cholelithiasis from cholecystitis since these two will often present with similar labs.
Table 1. Lab findings in various biliary tract conditions
Conditions that commonly present with jaundice and obstruct the common bile duct (choledocholithiasis and cholangitis) frequently have elevated bilirubin and alkaline phosphatase. Conditions due to inflammation and infections (cholecystitis and cholangitis) can have derangements in the white blood cell count.
As with all laboratory evaluations, lab results must be taken as whole and interpreted based on the patient’s presentation and other findings. Presence or absence of a single lab value must not be given undue considerations in management decisions. This is, as shown in the chart above, particularly true of the white blood cell count. Absence of an elevated white blood cell count does not rule out any of these conditions.
Diagnostic Imaging
Imaging studies are the mainstay of diagnosis of biliary tract diseases. Ultrasound (US) and CT are common modalities for initial workup of these entities, while endoscopic retrograde cholangiopancreatography (ERCP), magnetic resonance cholangiopancreatography (MRCP), and hepatobiliary iminodiacetic acid (HIDA) scans serve to further confirm and, in the case of ERCP, treat these conditions.
Ultrasound
Ultrasound is the initial diagnostic study of choice for biliary tract diseases. It is a low risk, non-invasive procedure that is generally readily available. Ultrasound can be an accurate modality at identifying cholelithiasis when performed by credentialed ED practitioners at bedside. This is diagnosed by the presence of potentially mobile echogenic material within the gallbladder that casts deep shadows (Picture 1).
Gallstones outside of the gallbladder, however, may be missed by US which is significantly less sensitive (<80%, though much lower in many studies) for choledocholithiasis. Dilation of the common bile duct, which is diagnosed as > 6mm in adults up to age 60 and and additional +1 mm for each additional decade indicates the likely presence of biliary duct stone or other obstruction and may be seen in choledocholithiasis and cholangitis.
The sensitivity and specificity of ultrasound for acute cholecystitis is estimated to be between 88-94% and 78-80%, respectively. Ultrasonographic findings of cholecystitis include the presence of gallstones, gallbladder wall thickening (greater than 3mm), pericholecystic fluid, and a positive sonographic Murphy sign (maximum tenderness with pressure from the US transducer directly over the gallbladder). Distention of the gallbladder and increased blood flow to the gallbladder on Doppler studies can also be seen. Studies vary widely on the predictive utility of each individual finding on abdominal US for cholecystitis, but most agree that the presence of multiple findings increases the overall predictive value.
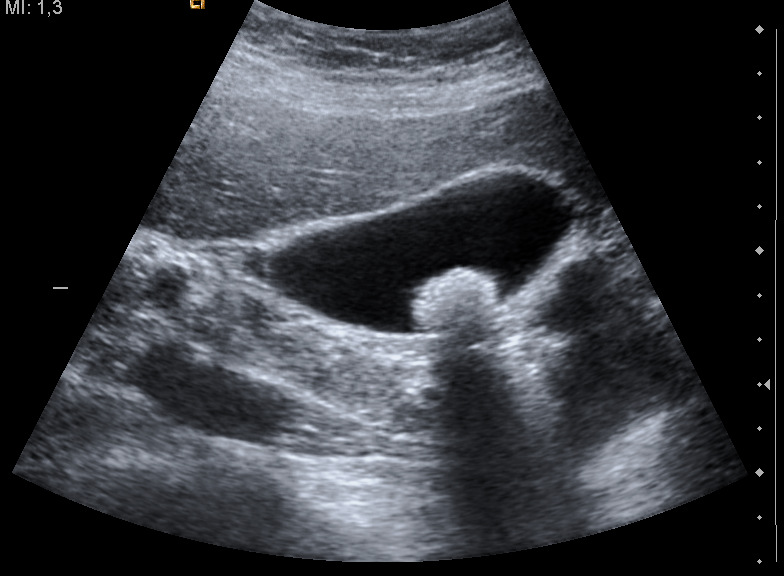
Image 1: Ultrasound showing echogenic 2 cm gallstone (blue arrow) with shadowing “comet tail” Source: Wikimedia Commons, Nevit Dilmen, used with permission
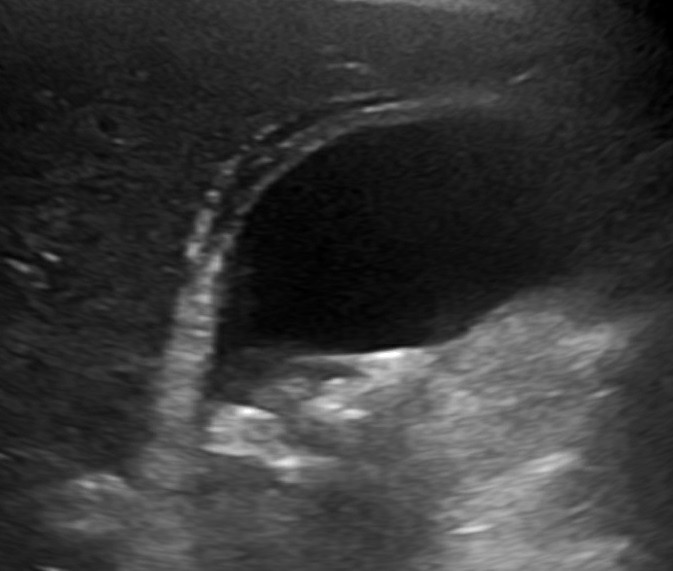
Image 2: US showing pericholecystic fluid (blue arrow) with stones in the bottom of the image
Source: Wikimedia Commons, Mikael Häggström, M.D., used with permission
CT Imaging
CT imaging is one of the most common initial modalities used for the evaluation of abdominal pain in the Emergency Department and plays an important role in the diagnosis of biliary disease.
CT imaging is less sensitive (<70%) than US for cholelithiasis, since many gallstones are radiolucent.
It is sensitive (92%) for the detection of acute cholecystitis due to its ability to detect gallbladder distension, wall thickening, and pericholecystic fluid. CT may outperform ultrasound in the detection of rare complications of acute cholecystitis such as emphysematous cholecystitis or GB perforation.
It is highly sensitive (>96%) for detecting biliary obstruction as seen in choledocholithiasis and cholangitis.
In most cases, ultrasound will be preferred over CT for initial evaluation due to its lower risk and higher sensitivity for detecting stones. However, if US results are equivocal, a HIDA scan is not readily available, or a broad differential to the patient’s abdominal pain is still being considered, a CT scan in the Emergency Department is reasonable.
Hepatobiliary Imino-Diacetic Acid (HIDA) Scan
HIDA scan is 90-94% sensitive for the presence of acute cholecystitis and is indicated if US is equivocal or negative for cholecystitis in the presence of a high clinical suspicion.
A HIDA scan is a nuclear imaging procedure that utilizes a radioactive tracer (technetium-99m) to evaluate gallbladder function. The tracer is injected intravascularly, circulates to the liver, and is excreted into the biliary system. A normal (or negative) HIDA is visualization of the gallbladder within 1 hour of tracer injection. Lack of visualization of the gallbladder within 4 hours after the injection constitutes a positive study and indicates the presence of cholecystitis or cystic duct obstruction.
Common drawbacks to the use of HIDA scan in the ED are that the scan performs more poorly if the patient has eaten within the last 24 hours and that it requires a long period of monitoring after tracer infusion (up to 4 hours).
Endoscopic Retrograde Cholangiopancreatography (ERCP) / Magnetic Resonance Cholangiopancreatography (MRCP)
ERCP has long been considered the gold standard for diagnosis of obstructive duct pathology such as choledocholithiasis. ERCP is used to both diagnose and treat diseases of the biliary and pancreatic ducts. In this technique an endoscope is passed through the GI tract into the biliary system. Fluoroscopy allows visualization of dye injected into the biliary tree and obstructions can be identified. During dilation of the Sphincter of Oddi and installation of dye, many obstructions will resolve. This is an invasive procedure associated with significant risks including pancreatitis (~5%), perforation of the GI tract or ductal system, dye reactions, and bleeding. Due to these risks, its use strictly for diagnosis is decreasing as less invasive diagnostic studies such as MRCP and endoscopic ultrasound become more widely available.
MRCP has the advantage of being highly accurate (both in sensitivity and specificity) when compared to ERCP and does not expose patients to an invasive procedure, contrast dye, or the documented complication, morbidity, and mortality rates ERCP carries. MRCP can now be used to ensure that ERCP is reserved mainly for patients in need of therapeutic ERCP.
Treatment
Episodes of biliary colic associated with cholelithiasis are typically self-limited and should be treated symptomatically with antiemetics, fluids, and appropriate pain control (NSAIDs and/or opioids). Medical treatments such as ursodeoxycholic acid and chenodeoxycholic acid (both of which inhibit hepatic secretion of biliary cholesterol and promote dissolution of gallstones) are available but not used as they are ineffective. Extracorporeal shock wave lithotripsy (similar to what is done in renal stones) is a rarely performed procedure meant to break up stones in the gallbladder, often in conjunction with post procedure ERCP. These are reserved for patients who are not operative candidates. The definitive treatment for symptomatic cholelithiasis is surgical removal of the gallbladder (cholecystectomy). Patients may benefit from dietary changes (low fat foods) until their operation.
Choledocholithiasis is treated with surgical or endoscopic (ERCP) removal of the stone.
Initial treatment of cholecystitis and cholangitis is the same as for biliary colic – symptom control with fluids, antiemetics and analgesics. In addition, broad-spectrum parenteral antibiotics should be administered early. Antibiotic selection in both conditions should cover for enteric gram negatives and anaerobes. In mild cases, a cephalosporin such as ceftriaxone with metronidazole (for anaerobic coverage) is adequate. In moderate to severe cases, piperacillin-tazobactam or meropenem as single agents are reasonable. Vancomycin is generally reserved for postoperative infections.
Prompt surgical consultation is imperative. Cholecystectomy is indicated in cholecystitis, but may be delayed, especially in the critically ill patient. ERCP +/- sphincterotomy may be performed in cases of cholangitis believed to be due to an obstructing stone in the common bile duct. In critically ill patients, surgical or percutaneous decompression (cholecystostomy) with a biliary drain may be considered in both conditions.
Pregnant patients with cholelithiasis should be managed symptomatically until after pregnancy. Pregnant patients with cholangitis should be managed the same as non-pregnant patients (parenteral antibiotics and early biliary drainage) with the exception of using pregnancy-safe antibiotics (avoid fluoroquinolones). Pregnant patients in their first or second trimester with acute cholecystitis will likely undergo cholecystectomy. Pregnant patients in their third trimester with acute cholecystitis are generally trialed with nonoperative management to postpone cholecystectomy to the postpartum period due to higher complication rates.
In patients with acute pain caused by these conditions and whose pain is controlled by NSAIDs, morphine is a reasonable narcotic option for pain control. The peristalsis and pressure of the Sphincter of Oddi is exquisitely sensitive to all narcotics however, no other narcotic (including meperidine) has been shown to be superior to morphine in any outcome-based studies in biliary disease for pain control. Morphine is advantageous in that it is widely available, familiar, and lasts longer than most other available opiates. Compared with meperidine, specifically, other opioids have less seizure risk.
Disposition
Patients with biliary colic whose symptoms are improving may be discharged home with outpatient referral to a general surgeon for consideration of an elective cholecystectomy. They should be advised to return immediately for signs of complications of gallstones such as prolonged symptoms (> 6 hours), and/or symptoms associated with fever (> 100.4° F) or jaundice.
Most patients with choledocholithiasis should be admitted for definitive treatment due to high rates of associated complications such as cholangitis, pancreatitis, gallbladder perforation and gangrene.
All patients with acute cholecystitis and cholangitis must be admitted to the hospital for IV antibiotics and possible surgical intervention. In the presence of signs of sepsis, end organ dysfunction, or hypotension, ICU admission may be required.
Pearls and Pitfalls
Obtain a full history and physical, paying close attention to the duration of pain (>6h).
Remember that associated symptoms such as fever or jaundice are signs of more serious biliary pathology such as cholecystitis or cholangitis.
Murphy sign is a specific maneuver, not just RUQ pain to palpation; the patient should have cessation of inhalation during palpation. However, an ultrasonographic Murphy sign is where the patient has maximal pain when pressure is exerted from the transducer probe immediately over the gallbladder.
A CBC, LFTs, and lipase are routine labs ordered in the evaluation of biliary tract pathology.
Ultrasound is the preferred initial imaging modality and is highly sensitive and specific for stones.
Patients with uncomplicated biliary colic can follow up in clinic with symptomatic control and dietary modification.
Broad spectrum antibiotics and fluid resuscitation should be given to patients with cholecystitis and cholangitis, particularly if showing signs of sepsis on presentation.
Early surgical consultation is important for cholecystitis and cholangitis.
Case Resolution
Two large bore IVs are placed, and the patient is given fluid resuscitation and pain control. Broad spectrum antibiotics are administered. Charcot triad is identified and leads to the suspicion of biliary pathology – specifically cholangitis. An US performed at bedside shows multiple gallstones without gallbladder wall thickening, pericholecystic fluid, or sonographic Murphy sign, but the common bile duct measures at 10 mm. General surgery is emergently consulted and the patient is admitted. An MRCP performed later that day confirms common bile duct obstruction, and an ERCP is performed with passage of the stone and improvement in symptoms. The patient subsequently undergoes a laparoscopic cholecystectomy to prevent recurrence.
References
- Bennett GL and Blathazar EJ. Ultrasound and CT evaluation of emergent gallbladder pathology. Radiol Clin North Am 2003;41:1203-1216.
- Csendes A et al. Simultaneous bacteriologic assessment of bile from gallbladder and common bile duct in control subjects and patients with gallstones and common duct stones. Arch Surg. 1996; 131(4):389.
- Gore RM, Yaghmai V, Newmark GM, et al. Imaging benign and malignant disease of the gallbladder. Radiol Clin North Am 2002;40:1307-1323.
- Jain A et al. History, Physical Examination, Laboratory Testing, and Emergency Department Ultrasonography for the Diagnosis of Acute Cholecystitis. Acad Emerg Med 2017 Mar;24(3):281-297
- Kendall JL, Shimp RJ. Performance and interpretation of focused right upper quadrant ultrasound by emergency physicians. J Emerg Med. 2001;21:7-13.
- Moscati RM. Cholelithiasis, cholecystitis, and pancreatitis. Emerg Med Clin North Am 1996;14:719-737.
- Ralls PW, Colletti PM, Lapin SA, et al. Real-time sonography in suspected acute cholecystitis. Prospective evaluation of primary and secondary signs. Radiology. 1985;155:767-771.
- Saini S. Imaging of the hepatobiliary tract. N Engl J Med 1997;336:1889-1894.
- Singer AJ, McCracken G, Henry MC, et al. Correlation among clinical, laboratory, and hepatobiliary scanning findings in patients with suspected acute cholecystitis. Ann Emerg Med 1996;28:267-272.
- Strasberg SM. Acute calculous cholecystitis. NEJM 2008; 358: 2804-11.
- Trowbridge RL, Rutkowski NK, Shojania KG. Does this patient have acute cholecystitis? JAMA 2003;289:80-86.
