Appendicitis
Author: Matthew Fannell MD, John Solms MD, J. Scott Wieters MD, Texas A&M College of Medicine, Baylor Scott & White Hospital
Editor: Eric Blazar, Inspira Vineland Medical Center, Rowan School of Medicine, 2019
Last updated: November, 2019
Case Study
19 year old male presents with 2 day history of intermittent right lower quadrant abdominal pain. He reports that the pain has progressively worsened and has slowly moved from just below his belly button and it now more intense in the right lower quadrant. Also reports that the pain is made worse by walking and by the car ride to the ED. He complains of one episode of vomiting and intermittent nausea. No other significant medical history. On exam VS are Temp 100.4, HR 95, RR 18, BP 110/73 SpO2 99% on RA. Patient appears uncomfortable and is sitting quietly on the stretcher. Exam is pertinent for tenderness over the right lower quadrant of the abdomen with rebound tenderness. No other abnormal findings on exam.
Objectives
Upon completion of this module, the student will be able to:
- Identify patients with suspected appendicitis
- Describe the classic history and physical exam findings in appendicitis, as well as atypical presentations
- Discuss the roles of laboratory tests and imaging in the diagnosis of appendicitis
- Describe the management options for appendicitis
Introduction
Acute appendicitis is one of the most common atraumatic surgical emergencies. It can affect patients at any age, however the incidence peaks around the second and third decades of life. Reports of male to female predominance are conflicting, with some sources citing either sex with a slight majority. In pregnancy, appendicitis is the most common non-obstetric surgical emergency. Although the incidence peaks earlier in life, appendicitis can present at any point in life. Thus, the diagnosis should be considered in patients of all ages with atraumatic abdominal pain.
Initial Actions and Primary Survey
As with any patient presenting to the ED, the primary survey should precede all other management. A vast majority of patients who ultimately are diagnosed with appendicitis present with stable vital signs and airway, breathing, and circulation intact. However, any compromise in these areas must be addressed first. If necessary, resuscitation should begin with IV fluids to treat hypotension and antipyretics to treat fever. Pain should also be adequately managed
Presentation
The classic presentation of appendicitis occurs as follows:
- Vague epigastric or periumbilical pain.
- Nausea, vomiting and anorexia.
- Abdominal tenderness, migrating and then localizing to the right lower quadrant.
- Fever
- Leukocytosis
This classic presentation though, is highly variable, especially at the extremes of age and due to the anatomical variation of appendix location. A retrocecal appendicitis may present a variety of ways including low back pain, left sided pain and even right upper quadrant pain.
Right lower quadrant pain and guarding generally have a high sensitivity (81%) for appendicitis, but are poorly specific (53%). Abdominal rigidity is also highly specific (83%) but has a low sensitivity (27%). The classic Psoas, Obturator and Rosving’s signs are all relatively poor predictors of appendicitis. No single exam finding should be used to rule in or rule out the disease.
Atypical presentations can occur in any patient, but more are more likely in extremes of age, and pregnant patients. Children can be more of a diagnostic challenge due to communication barriers and vague symptoms. In children less than four years old perforation rates can be as high as 90%.
Another high-risk population includes elderly patients presenting with subtle signs and significant comorbidities. They too can often present late. Immunosuppressed patients will likely have a decreased inflammatory response and may have more subtle signs, similar to the elderly population.
Maintaining a high level of suspicion for appendicitis is important. However, it is vital to consider a broad differential as well. A genital exam is paramount in both sexes. A testicular exam should be performed in males to evaluate possible torsion or other male GU etiology that would present with RLQ abdominal pain. Females of childbearing age require special attention to rule out gynecologic or obstetric pathology that can be misdiagnosed as appendicitis. These disease etiologies include ectopic pregnancy, ovarian torsion, and tubo-ovarian abscess. The pregnant patient can also have atypical complaints secondary to a gravid uterus.
Diagnostic Testing
Laboratory Studies
There is no single lab test specific for the diagnosis of appendicitis. Many patients with appendicitis will have leukocytosis, however, 10-20% of patients will have a normal white blood cell count. The converse is also true. Many patients with leukocytosis will not have appendicitis, as many other pathologies cause an elevated WBC. Another inflammatory marker, C-reactive protein, can be used along with the WBC for supporting or ruling out appendicitis CRP alone cannot be used to rule in or rule out the disease1. Both an elevated CRP and WBC have a combined sensitivity of 98%, and if both labs are within normal limits the diagnosis is less likely.
Urine studies should be obtained. They are useful for determining pregnancy, and evaluating for infection and hematuria. Pyuria without bacteria present can be cause by inflamed appendix in close proximity to the ureter or bladder. Hematuria without other findings could suggest a ureteral stone as the cause of pain. Again, UA in isolation cannot rule out appendicitis.
Ultrasound
Ultrasound is quickly becoming a more popular diagnostic tool in the Emergency Department. It is the preferred imaging modality in children and pregnant patients with suspected appendicitis due to the absence of radiation. One multicenter cohort study found ultrasound to be 72.5-86% sensitive and 96% specific for appendicitis in children. The diagnostic accuracy is variable depending on the skills of the sonographer and size of the patient. Ultrasound is typically much less sensitive in adults than children. A normal appendix on ultrasound is typically less than 6 mm and compressible. An appendix greater than 6-7 mm in diameter and noncompressible is indicative of appendicitis. Other findings that support the diagnosis are increase wall thickness, fecalith, and increased vascularity. Doppler flow can be used to demonstrate the increased vascularity of an inflamed appendix. An excellent resource for learning this skill is the Ultrasoundpodcast.com. (http://www.ultrasoundpodcast.com/2011/08/appendix/)
Computed Tomography
CT is currently the preferred imaging study for evaluating acute appendicitis in adult males and nonpregnant females. CT of the abdomen/pelvis is also more useful for evaluating alternative diagnoses, and diagnosing complications of appendicitis (perforation, abscess, etc.). As with ultrasound, an enlarged appendix over 6-7 mm, increased wall thickness, fecalith, and peri-appendiceal stranding can support the diagnosis. The overall sensitivity for IV contrast enhanced CT ranges from 95-100%, which is considerably better than ultrasound. Similarly, specificity is around 96%. One study showed that non–contrast CT (90 % sensitivity and 86% specificity) was inferior to CT with rectal only administered contrast (93% sensitivity and 95% specificity) and CT with both IV and oral contrast (100 % sensitivity and 89% specificity). However, given the slight increase in morbidity associated with oral and rectal contrast, along with improved resolution of newer CT scanners, most clinicians use IV contrast alone. While IV contrast is recommended for evaluation of suspected appendicitis, non-contrast CT still has excellent sensitivity, ranging from 89.5%-96% depending on the study. The ability to accurately use non-contrast CT studies is helpful in patients with relative contraindications, such as renal insufficiency and contrast allergy. Non-contrast CT scans are also quicker to obtain.
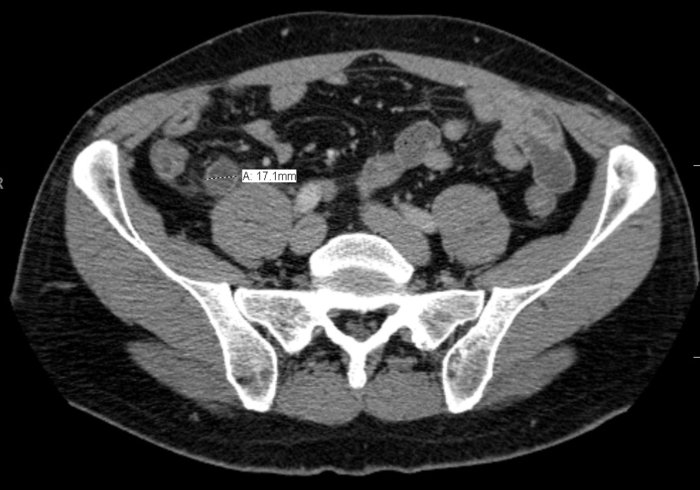
Image 1. CT image of appendicitis demonstrating a dilated appendix with periappendiceal stranding. Original image provided by J. Scott Wieters MD. Attribution 4.0 International (CC BY 4.0)
Magnetic Resonance Imaging
Utilizing MRI to diagnose appendicitis is typically reserved for pregnant patients after a non-diagnostic ultrasound. MRI has a similar diagnostic accuracy compared to CT, however emergent MRI often has limited availability, is expensive, and is more time consuming. As with ultrasound, MRI avoids radiation exposure however, the contrast medium used in the study, IV gadolinium, is a potential teratogen. Similar to using IV contrast with CT, IV gadolinium is not traditionally used in patients with renal insufficiency.
How to make the Diagnosis?
As mentioned above most cases of suspected appendicitis require lab test and imaging.
- In adults, complete blood count, basic metabolic panel, CRP, and urinalysis are a good starting point. Urine pregnancy should be obtained for all females of childbearing age.
- If the patient is a male or a nonpregnant female a CT scan would be the imaging modality of choice, preferably with IV contrast.
- If the patient is child, pregnant or you have a high suspicion for gynecologic disease, then ultrasound would be a more appropriate initial imaging modality.
- For low risk pediatric patients with an indeterminate ultrasound observation for serial exams is warranted to avoid radiation and/or contrast. Another reasonable option in a low risk patient would be to have them return to the emergency department in 12 to 24 hours for a repeat examination. This option to return is also applicable to patients with negative CT scans and persistent symptoms.
All patients discharged home after a negative workup should be counseled on very specific return precautions. No diagnostic test is perfect.
Clinical decision tools, such as the Alvarado score can be useful when considering the diagnosis of appendicitis. A calculator for the Alvarado score can be found here. A low score, <1-4, has approximately 96% sensitivity for ruling out appendicitis. In a meta-analysis the Alvarado score was inconsistent in children, tended to over predict appendicitis in women, but was well calibrated in adult males.
Treatment
Acute appendicitis is traditionally treated surgically. Prompt appendectomy has been the standard treatment for decades. That said, there have been recent studies that call into question the reliance upon surgery for uncomplicated appendicitis given the morbidity associated with open appendectomy. In settings where laparoscopic technology exists, such as the vast majority of the United States, consensus remains that surgical intervention is superior; however, in resource limited settings there are compelling studies that suggest that IV antibiotics, or even in some cases oral antibiotics, can produce sufficient success in treatment to overcome the risk associated with open appendectomy. At this time, studies with greater power are needed for broad application of an antibiotics first approach. RebelEM non-operative treatment of appendicitis. Skeptics Guide to EM non-operative treatment of pediatric appendicitis. Of note, certain complicated cases like perforation with a walled off abscess may require drainage by interventional radiology. Decision making in these scenarios should be discussed with an interdisciplinary team for coordination of care.
Once the diagnosis is confirmed the patient should be made NPO and IV antibiotics should be started in the emergency department. Examples of appropriate antibiotics for uncomplicated appendicitis include ampicillin-sulbactam, or cefoxtin, or a combination of metronidazole and ciprofloxacin.
For complicated appendicitis (perforation, abscess, immunocompromise, etc.) a carbapenem, such as meropenem or imipenem, can be used or an extended spectrum penicillin with a beta-lactamase inhibitor, such as piperacillin/tazobactam.
Do not forget IV fluid resuscitation, pain control and antiemetics. Analgesia with reasonable doses of opioids has not been shown to alter the abdominal exam.
Emergency Department Disposition
- OR for appendectomy
- Interventional Radiology for percutaneous drainage of abscess
- Observation in hospital for serial examinations
- Return in 12-24 hours for a repeat examination
Case Resolution
Patient is treated with IV morphine, ondansetron, and 1 liter Lactated Ringers bolus. Labs demonstrate an elevated WBC to 13.9k. CT of the abdomen/pelvis demonstrates an inflamed appendix with stranding in the right lower quadrant consistent with uncomplicated appendicitis. No evidence of perforation. A single dose of cefoxitin was administered and the on-call surgeon was consulted for surgical removal. Patient had an unremarkable operative course and was discharged home later that evening.
Pearls and Pitfalls
- Maintain a broad differential diagnosis
- An afebrile patient with a normal WBC does not rule out appendicitis
- There is no single sign, symptom, or lab that completely rules out appendicitis
- Urinalysis with pyuria or hematuria can be appendicitis due to an inflamed appendix next to the bladder and hematuria may represent nephrolithiasis. .
- The localization of pain can be atypical due to the anatomic position of appendix and referred pain.
- Ultrasound should be used as the first imaging study in children and pregnant females
- Extremes of age have atypical presentations necessitating a high index of suspicion
- In females presenting with RLQ pain and tenderness, make sure gynecologic diseases have been appropriately considered including ectopic pregnancy, ovarian torsion, or tubo-ovarian abscess.
- Check the testicles! Do not miss torsion.
- Every patient discharged home after a negative workup should receive appropriate return precautions. No test is perfect.
- Please see additional pearls and pitfalls here
References
- Sengupta A, Bax G, Paterson-Brown S. White cell count and C-reactive protein measurement in patents with possible appendicitis. Ann R Coll Sure Engl. 2009;91(2):113-115.
- Anderson, BA et al. Am J Surg. 2005 Sep;190(3):474-8. A systematic review of whether oral contrast is necessary for the computed tomography diagnosis of appendicitis in adults.
- Cope, Z; Silen, WCope’s Early Diagnosis of the Acute Abdomen (22nd ed.). New York: Oxford University Press. 2010. ISBN 978-0-19-973045-2. p. 67 – 104.
- Dearing, Daniel & A Recabaren, James & Alexander, Magdi. Can Computed Tomography Scan be Performed Effectively in the Diagnosis of Acute Appendicitis without the Added Morbidity of Rectal Contrast?. The American surgeon. 2008. 74. 917-20.
- DeKoning, E. Acute Appendicitis. Chapter 84. In: Tintinalli J, ed. Emergency Medicine Medicine: A Comprehensive Study Guide. 7th ed. McGraw-Hill; 2011:574-78.
Hlibczuk, V et al. Ann Emerg Med. 2010 Jan;55(1):51-59.e1. doi: 10.1016/j.annemergmed.2009.06.509. Diagnostic accuracy of noncontrast computed tomography for appendicitis in adults: a systematic review. - Humes, D and Simpson, J. Clinical review: Acute appendicitis. BMJ 2006;333;530-534. doi:10.1136/bmj.38940.664363.
- Kharbanda, A and Sawaya, R. Acute Abdominal Pain in Children. Chapter 124. In: Tintinalli J, ed. Emergency Medicine Medicine: A Comprehensive Study Guide. 7th ed. McGraw-Hill; 2011:839-845.
- Mittal, MK et al. Performance of ultrasound in the diagnosis of appendicitis in children in a multicenter cohort. Acad Emerg Med. 2013 Jul;20(7):697-702. doi: 10.1111/acem.12161
- Ohle, R. BMC Medicine. 2011, 9:139 doi:10.1186/1741-7015-9-139. The Alvarado score for predicting acute appendicitis: a systematic review
- Salminen, Paulina et al. “Five-Year Follow-up of Antibiotic Therapy for Uncomplicated Acute Appendicitis in the APPAC Randomized Clinical Trial” JAMA vol. 320,12 (2018): 1259-1265.
- Smith, MP et al. Expert Panel on Gastrointestinal Imaging. ACR Appropriateness Criteria right lower quadrant pain–suspected appendicitis. [online publication]. Reston (VA): American College of Radiology (ACR); 2013.
- Talan, David A et al. “Antibiotics-First Versus Surgery for Appendicitis: A US Pilot Randomized Controlled Trial Allowing Outpatient Antibiotic Management” Annals of emergency medicine vol. 70,1 (2016): 1-11.e9.
