Breathing
Author Credentials
Case Study
A 37-year old male with a history of obstructive sleep apnea presents to your emergency department with a recurrent anterior shoulder dislocation. Your initial attempts at closed reduction have been unsuccessful. You proceed with procedural sedation utilizing
propofol, for which the patient has tolerated in the past, and it is quickly reduced with gentle traction. Immediately after the reduction is completed, end tidal waveform capnography demonstrates apnea, and the patient is gradually becoming hypoxic.
Despite supplemental oxygen, his oxygen saturation drops from the high 90s into the 70s. Noxious stimulation elicits minimal effect on respirations; the nurse looks nervously at you for guidance. What are your next steps?
Objectives
By the end of this module, the student will be able to:
To understand the mechanisms by which breathing can become compromised, and which interventions may be helpful.
To describe the mechanics of bag-valve mask ventilation, its indications and limitations.
To understand and describe non-invasive positive pressure ventilation (NIPPV) and its utilization in the Emergency Department.
Introduction
Respiratory distress often results from either a failure of the patient’s airway (covered in another section) or their inability to breathe. Problems with breathing can be further broken down into issues with either oxygenation or ventilation. Understanding which of these functions is compromised will allow the emergency physician to choose specific interventions that are appropriate. It will also help them to quickly identify those interventions that may not work.
Ventilation is the process of moving air in and out of the lungs, driven by changes in intrathoracic pressure. Proper ventilation allows for oxygen-rich air to enter the lungs and oxygen-deprived, CO2-rich air to exit. The process relies upon a functioning circuit of thoracic musculature, bony stability and diaphragmatic strength. Diseases that affect the body’s ability to move air successfully (e.g. pneumothorax, flail chest) will ultimately cause difficulties in respiration.
While oxygen transportation and delivery to body tissue is a complex and multi-system process, it begins with the diffusion of oxygen-rich air over the alveoli to the pulmonary capillaries. Any disease process that affects molecular diffusion across the lung tissue (e.g. pneumonia, Acute Respiratory Distress Syndrome (ARDS)) will affect oxygenation and eventually cause the patient to develop respiratory difficulty. Disease processes that lead to respiratory failure will be discussed in a separate section.
Bag-Valve-Mask Ventilation
Often called assisted ventilation, bag-valve-mask (BVM) ventilation is manually applied positive pressure ventilation delivered directly to a patient’s airway. BVM ventilation is performed via a plastic, well-fitting mask applied to a patient’s face (see Figure 1). Bag-valve ventilation may also be accomplished through an endotracheal tube (ETT) inserted directly into the patient’s trachea, or a supraglottic device such as a laryngeal mask airway (LMA). Properly performing bag-valve ventilation is a difficult skill, but one which may be life saving, and should be mastered by all emergency medicine clinicians.

Figure 1. Bag Valve Mask (Figure 1) The BVM consists (from left to right) of a mask which fits on the face, a valve which allows only one way flow of oxygen, a bag for pumping the air forward and an oxygen reservoir (Photo courtesy of Alex Maybury, MD. Used with permission.)
Often the most critical and difficult step in BVM ventilation is to ensure the application of a well-sealed, well-fitting mask to a patient’s face. Difficulty may be encountered in patients with altered anatomy, dentures, facial hair or obesity. Walls, et al published the mnemonic MOANS to help emergency providers predict which patients may be difficult to ventilate with BVM.
- Mask Seal (trauma, blood, beards)
- Obesity
- Age (>55)
- No teeth (leave dentures in)
- Stiff (lungs, neck)
BVM ventilation, whenever possible, should be performed by two providers. One provider uses both hands to apply the facemask, focused on maintaining an adequate seal, while a second provider squeezes the self-inflating bag to deliver oxygen-rich air to the patient and provide gas exchange. One-handed ventilation may be performed if necessary, but difficulty is often encountered establishing and maintaining an adequate seal. BVM ventilation may be optimized by placing an oral airway or nasal airway, which may alleviate the physical obstruction caused by redundant tissue or a large tongue.
The facemask should rest on the bridge of the nose, extend over the malar eminences, with the base extending to the mandibular alveolar ridge. In some situations it may be prudent to add or remove air from the mask itself using a syringe.
Below is an excellent video describing how to effectively perform BVM ventilation:
Two-provider BVM ventilation
To perform “two-provider” BVM ventilation, one clinician’s sole role is applying and optimizing mask seal, while the second squeezes the bag to appropriately ventilate. The first clinician should place themselves at the head of the bed. Utilizing the pads of the thumb and index finger of each hand, a “C” is made upon the mask to apply equally distributed downward pressure, securing it to the patient’s face. The remaining digits are used to lift the mandible towards the facemask (“E”). The provider’s hands should form an “E-C shape” and provide a tight seal between the facemask and patient’s face (see below).

Figure 2. Two-provider, two-handed bag valve mask technique, aka “the E-C grip” (Photo courtesy of Alex Maybury, MD. Used with permission.)
An alternate position is resting the clinician’s thenar eminences over the lateral aspect of the mask, while the mandible is lifted toward the mask itself, using the free digits to perform a chin lift or jaw thrust maneuver (see below). Care is taken in either techniques to use bony prominences to obtain mechanical advantage, rather than compressing soft tissue, which may obstruct and otherwise impair ventilation. In both techniques, the second provider stands to the side of the patient and squeezes the self-inflating bag to deliver oxygen at a clinically indicated respiratory rate.

Figure 3. Two-provider, alternate two-handed bag valve mask technique (Photo courtesy of Alex Maybury, MD. Used with permission.)
One-provider BVM ventilation
In single-provider BVM ventilation, the same clinician holds a face mask seal, tries to support a patent airway, and squeezes the self-inflating bag to deliver oxygen to the patient simultaneously. Using their non-dominant hand, the provider grasps the face mask with their thumb and index finger, forming a C-shape around the ventilation port. The web space between thumb and index finger may rest upon the mask for stability. Using the middle, ring and small finger of the same hand, the jaw and face is lifted towards the mask. If the provider’s hands are large enough, the small finger can be placed at the angle of the mandible to simultaneously perform a jaw thrust. Care must be taken not to compress the soft tissues under the tongue, as this may alter the mask seal or cause complete airway obstruction via the tongue.

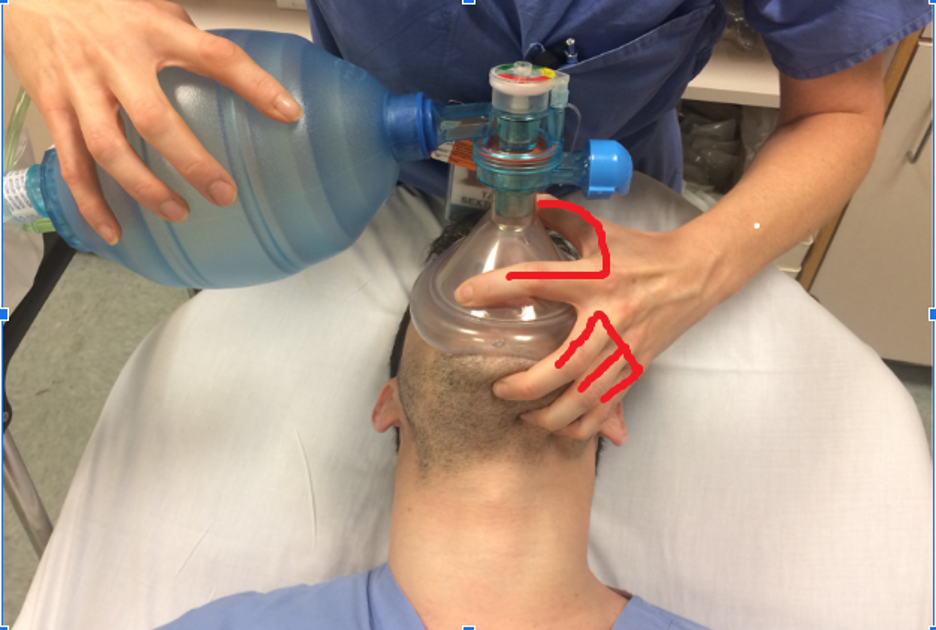
Figure 4. Single-provider, one-handed BVM technique using the E-C technique (Photo courtesy of Alex Maybury, MD. Used with permission.)
Providing ventilations
The provider should take steps to avoid overly aggressive BVM ventilation. Ideally, patients should receive 5-6 cc/kg per ventilation, or a tidal volume of 350 cc for a 70 kg patient. Starting respiratory rate should be 10-12 breaths/minute, which can be accomplished by the provider counting 5 to 6 seconds between each delivered breath.
Respiratory rate, tidal volume and other parameters should be adjusted to best support the specific patient as their disease process requires. All clinicians performing BVM ventilation via face mask should also remember that the delivered air can, and likely will, insufflate the stomach as well as the lungs, putting these patients at risk for vomiting and aspiration. Patients being ventilated via endotracheal tube have significantly less risk for aspiration, but remain at risk for pneumothorax or other sequelae of barotrauma.
Adequate ventilation can be assessed by watching for chest rise, by listening for air leaks around the face mask, and by auscultating for intrathoracic air exchange. If ventilation is not successful, the clinician should ensure that all equipment is functional,
the seal is tight and that adequate oxygen is being delivered via the BVM. Troubleshooting techniques include:
Changing the size of the mask
Inflating or deflating the mask with a syringe to improve the seal
Attempting a new bag-valve mask device
Adjusting the PEEP device on the BVM device
Applying lubricant to a beard to ensure a good mask seal
Insertion of oral or nasopharyngeal airways
Recruiting additional participants to help
Airway Adjuncts
Airway adjuncts, like the nasopharyngeal and oropharyngeal airways, help splint the airway open by pushing the tongue and airways out of the way to open the airway and facilitate successful BVM ventilation. These airway adjuncts can be especially helpful in the unresponsive patient, where the loss of muscle tone can cause the soft tissues and tongue to obstruct the airway.
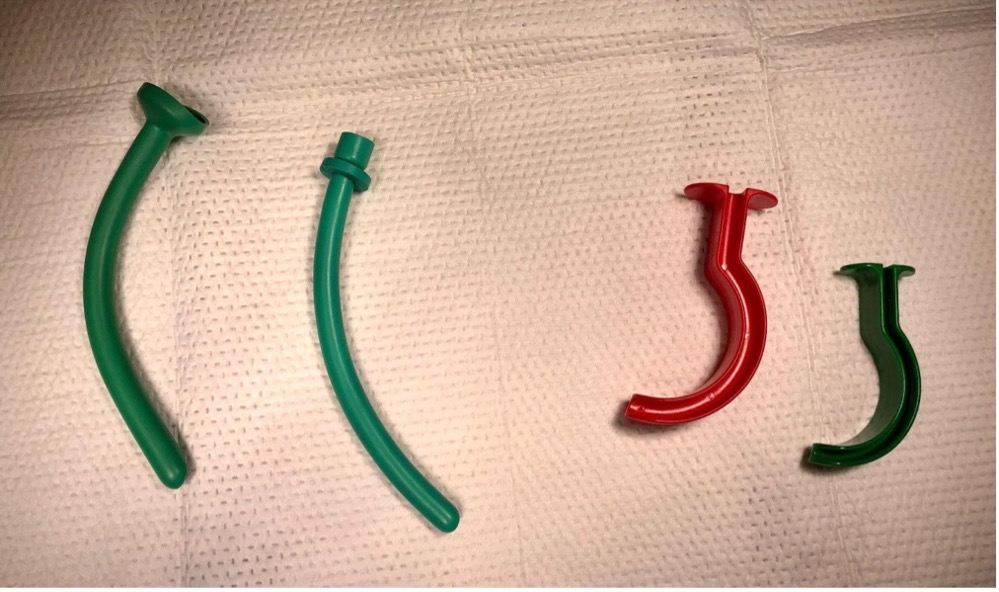
Figure 5. Nasopharyngeal airways (left) and orophayngeal airways (right) of varying sizes and styles (Photo courtesy of Alex Maybury, MD. Used with permission).
Nasopharyngeal airway
Colloquially known as a nasal trumpet, the nasopharyngeal airway (NPA) is a device used to enhance patency of the upper airway and promote ventilation. The NPA is a hollow rubber tube which is inserted into the naris and extends into the posterior pharynx, stenting open soft tissue and providing an adequate air passage for gas exchange. This can be placed in awake, sedated or unconscious patients alike, and is fairly well tolerated.
Choosing the correct size of a nasopharyngeal airway is crucial to splinting the airway open. A NPA of the correct size, when placed on the patient’s nose, should terminate at the earlobe (Figure 6).

Figure 6. An appropriately sized nasopharyngeal airway. Note that it starts at the nose and terminates at the earlobe. Image of courtesy of Navdeep Sekhon, MD. Image used with permission.
Insertion of an NPA is performed blindly, similar to nasogastric tube placement, by introducing a well-lubricated device into either nares and advancing along the nasal floor, until the flange is fully seated against the tip of the nose. Placement may
be assisted by gentle rotation of the device as it is advanced, following the natural curve of the NPA, and subsequent placement can be performed on the contralateral side.
Contraindications to NPA use include suspected basilar skull fractures and facial trauma, due to theoretical risk for misplacement, extremely young children due to their anatomical differences, and known coagulopathy, as epistaxis may occur.
Oropharyngeal Airway
Oropharyngeal airway devices (OPAs) are plastic devices consisting of a flange and a curved body with airway channels on either side. These devices are used to distract the tongue from the posterior pharynx and larynx in order to obtain a patent airway and relieve airway obstruction. These devices are noxious and not well tolerated in conscious patients, but are an essential tool in effective resuscitation. An OPA is contraindicated in awake, alert patients with a gag reflex, as it may lead to vomiting, aspiration, increased intrathoracic and intracranial pressures.
Selection of the correctly sized OPA is critical, as incorrect sizing may fail to alleviate obstruction and could promote further airway obstruction. This may be estimated by measuring the distance from the patient’s lips to the angle of the mandible against the OPA itself (Figure 7). Placement is achieved by distracting the tongue along the floor of the mouth with a finger or tongue depressor, and advancing the OPA along the tongue, following the curvature of the device. Successful placement will lead to markedly improved manual ventilation.
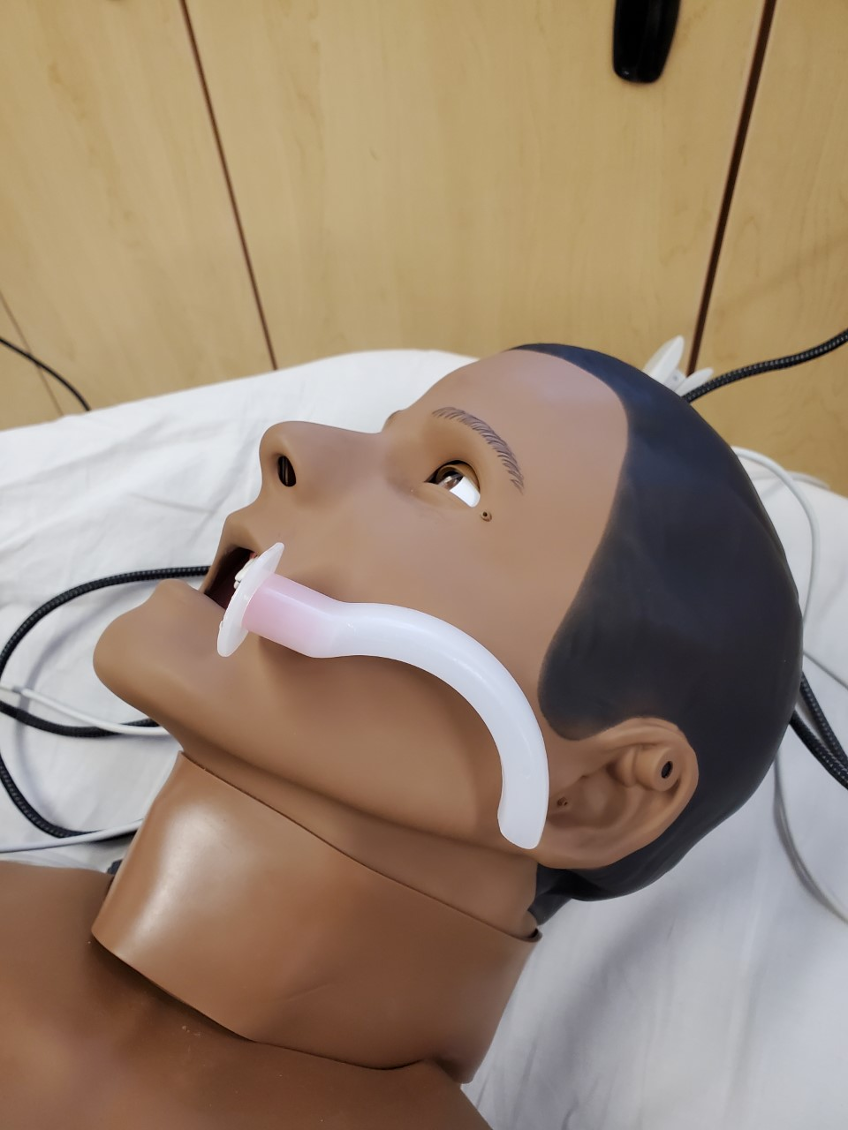
Figure 7. The appropriate size of an oropharyngeal airway, please note that it goes from the lips to the angle of the mandible. Image courtesy of Navdeep Sekhon, MD. Used with permission.
Below is an excellent video describing how to appropriately use nasopharyngeal and oropharyngeal airways:
Supraglottic Airways
Supraglottic airways are another way to help oxygenate and ventilate a patient using a bag valve mask. Supraglottic airways are devices that are actually placed into the mouth and rest above the glottis. An advantage of supraglottic airways is that they are designed to be blindly inserted to help with oxygenation and ventilation and can be placed quickly with minimal training.
It is important to note that supraglottic airways do not protect the airway. So, if you are worried at all about aspiration (if there is vomit or blood in the airway), a supraglottic airway would not be a good choice. Also, supraglottic airways can only be used on unresponsive patients as they can induce the gag reflex and vomiting.
A common type of supraglottic airway that is used in clinical practice is the laryngeal mask airway (LMA).

Figure 8. Laryngeal Mask Airway (LMA). Photo courtesy of Chrisjw37 and used under the Creative Commons Attribution 3.0 Unported license. Original image is located at: File:Laryngeal mask 100.jpg - Wikimedia Commons.
Below is an excellent video describing how to place a laryngeal mask airway:
Noninvasive Positive Pressure Ventilation
In patients with an adequate mental status and deteriorating respiratory status, Noninvasive Positive Pressure Ventilation (NPPV) can augment natural breathing by providing ventilator support through the delivery of pre-set volumes or pressures of air. Various methods of NPPV are available, including high-flow nasal cannula (HFNC), bilevel positive airway pressure (BiPAP) and continuous positive airway pressure (CPAP).
As indicated by its name, high-flow nasal cannula delivers oxygen via an augmented cannula placed under the nose. BiPAP and CPAP can be delivered either via a nasal mask or full-face mask (see below). HFNC and CPAP provide oxygen at continuous pressure (up to 15 cm of water for CPAP) while BiPAP allows for cyclical pressure changes. Inspiratory pressures (IPAP) for BiPAP can be started at 8-10 cm of water with expiratory pressures (EPAP) of 3-4 cm of water. Certain diseases will warrant modification of these settings from the outset. For example, patients with pulmonary edema typically start at IPAP of 15 with an EPAP of 5.
The positive pressure delivery of oxygen in both HFNC and BiPAP/CPAP allows for decreased work of breathing and increased total lung volume. Functional residual capacity increases, tidal volume goes up and minute ventilation goes up. The positive pressure drives fluid from intra-alveolar spaces into the extra-alveolar space, improving gas exchange across the alveoli. The ability to deliver positive pressure similar to those delivered via endotracheal intubation without the inherent risks of the intubation procedure itself, such as laryngeal and tracheal injuries, tube misplacement and complications from over and under-sedation, must also be considered.
Understanding the benefits and drawbacks to NPPV are important when deciding which patients are good candidates for this treatment modality. Patients who do well on NPPV usually suffer from an acutely reversible pulmonary condition, such as acute pulmonary edema or asthma.
HFNC is optimal in patients whose underlying cause of respiratory compromise is hypoxemia, rather than hypoventilation, though HFNC does provide a small amount of PEEP. Optimal candidates for all forms of NPPV are awake, alert and able to protect their airway.
Patients who suffer from claustrophobia or anxiety often do not tolerate the face mask, and therefore may not be ideal candidates for BiPAP and CPAP, however there are multiple mask choices that may improve their tolerance. Since NPPV does not provide the airway protection against aspiration or bleeding which endotracheal intubation does, it is not an appropriate choice in patients with a deteriorating or otherwise compromised airway.
NPPV allows the clinician an opportunity to ready other interventions which may address the underlying cause for respiratory distress. Medications such as nitroglycerin, albuterol, or steroids can be administered simultaneously while the patient’s oxygenation improves, and NPPV may thus be utilized as a bridge toward definitive therapy.
Side effects of NPPV are often related to the mask itself, as skin breakdown may occur when associated with long-term use. Excessive positive pressure via face-mask is no different than that delivered via endotracheal tube, as it may cause the same side effects as prolonged bag-valve ventilation or intubation: increased intrathoracic pressure, decreased venous return, leading to decreased blood pressure. The mask itself is tightly secured to the patient’s face in BiPAP or CPAP, and is thus contraindicated in an actively vomiting patient, and carries the risk of aspiration if a patient does begin vomiting. Prolonged positive pressure also places patients at risk for barotrauma and air trapping. Lastly, as discussed with BVM ventilation, excess air insufflation can cause gastric distension and possibly increase the risk of aspiration.
| Contraindications to BiPAP/CPAP |
| Uncooperative or Anxious Patient |
| Altered Mental Status |
| Inability to Protect the Airway |
| Facial Trauma |
| Pneumothorax |
| Epistaxis |
| Vomiting |
Table 1. Contraindications for BiPAP/CPAP

Pearls and Pitfalls
- Bag-valve mask ventilation is merely a bridge to definitive therapy: recovery or intubation.
- Adjuncts are your friend! NPA and OPAs make BVM easier in most scenarios, but be sure that you are using the correct size.
- Oral airways are contraindicated in conscious patients.
- Don’t use CPAP or BiPAP on an altered patient or on a patient who is apneic.
- Refrain from using benzodiazepines to help a patient who is anxious due to BiPAP or CPAP, as the resulting decrease in respiratory drive may result in respiratory collapse.
- For patients who are edentulous, leaving the dentures in while bagging the patient can be helpful to splint the lips to make it easier for the mask to maintain a seal.
Case Study Resolution
Your patient continues to desaturate despite noxious stimuli and supplemental oxygen via nasal cannula. You perform a jaw thrust with some improvement in oxygenation, and using your bag-valve mask, perform two-provider rescue breathing with improvement in oxygenation. A nasopharyngeal airway is placed to relieve his airway obstruction, and a few minutes later the patient resumes breathing spontaneously and removes the NPA himself. He is ultimately observed in the ED, fully recovers from his sedation, and a confirmatory radiograph is performed confirming successful reduction of his anterior shoulder dislocation. He is discharged after he is able to ambulate, and a family member has arrived to drive him home. The nurse pats your back and states, “Thanks for the save, doc!”
References
Atanelov Z, Aina T, Amin B, et al. Nasopharyngeal Airway. [Updated 2022 May 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513220/
Castro D, Freeman LA. Oropharyngeal Airway. [Updated 2022 Mar 3]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470198/
Masip J, Roque M, Sanchez B, et al: Noninvasive ventilation in acute cardiogenic pulmonary edema: systematic review and meta-analysis. JAMA 294: 3124, 2005. [PubMed: 16380593]
Nam KH, Kang HK, Lee SS, Park SH, Kang SW, Hwang JJ, Park SY, Kim WY, Suh HJ, Kim EY, Seo GJ, Koh Y, Hong SB, Huh JW, Lim CM. Effects of high-flow nasal cannula in patients with mild to moderate hypercapnia: a prospective observational study. Acute Crit Care. 2021 Aug;36(3):249-255. doi: 10.4266/acc.2020.01102. Epub 2021 Jul 26. PMID: 34311516; PMCID: PMC8435442.
Rescue breathing and bag-mask ventilation. Wenzel V, et al; American Heart Association; International Liaison Committee on Resuscitation. Ann Emerg Med. 2001 Apr;37(4 Suppl):S36-4
Walls RW, Manual of Emergency Airway Management. 4th ed. Lippincott, Philadelphia, PA 2012.
