Objectives
Upon finishing this module, the student will be able to:
- Recognize the presenting symptoms of pyloric stenosis
- Know the classic metabolic derangements for infants with pyloric stenosis
- Select the proper imaging study to diagnose pyloric stenosis
Introduction
Hypertrophic pyloric stenosis (HPS) occurs when thickening of the pylorus muscle leads to gastric outlet obstruction in young infants. It has an estimated prevalence of 1-2 per 1,000 infants, and is more common among males than females.1 The cause is unknown, although both genetic and environmental factors are thought to play a role. Infants less than 2 weeks of age who have taken either azithromycin or erythromycin are at increased risk for developing HPS.
Initial Actions and Primary Survey
Initial actions should include assessment of vital signs and hydration status. IV fluids should be given immediately if the child shows signs of shock or severe dehydration, and the child should be made NPO while awaiting further evaluation.
Presentation
HPS most commonly presents between 3 and 6 weeks of age. There may be a history of failure to thrive or poor weight gain. Infants often present with “projectile” vomiting. They may initially only vomit after some feeds, but vomiting progressively worsens over a period of days, until the infant begins to vomit after every feed. The emesis frequently looks like breast milk or formula. Infants continue to attempt to feed, and parents will generally report that the infant feeds vigorously but vomits shortly after. Peristaltic waves may sometimes be seen on exam, progressing from the left upper abdomen across to the right.
The classic finding on physical examination in infants presenting with pyloric stenosis was a palpable “olive” in the stomach, as the hypertrophied pylorus could be felt on exam. Infants also commonly presented with dehydration and electrolyte abnormalities caused by frequent vomiting, typically a hypokalemic, hypochloremic metabolic alkalosis. However, with many patients presenting and being diagnosed earlier, fewer patients have an olive palpated at diagnosis, and the majority do not have the classic electrolyte derangements at presentation.2
Diagnostic Testing
Diagnosis of pyloric stenosis is most commonly made by ultrasound. HPS is diagnosed when the pylorus has a thickness of greater than 3 mm and a length of greater than 14 mm (see image below) with no passage of gastric contents into the small intestine.
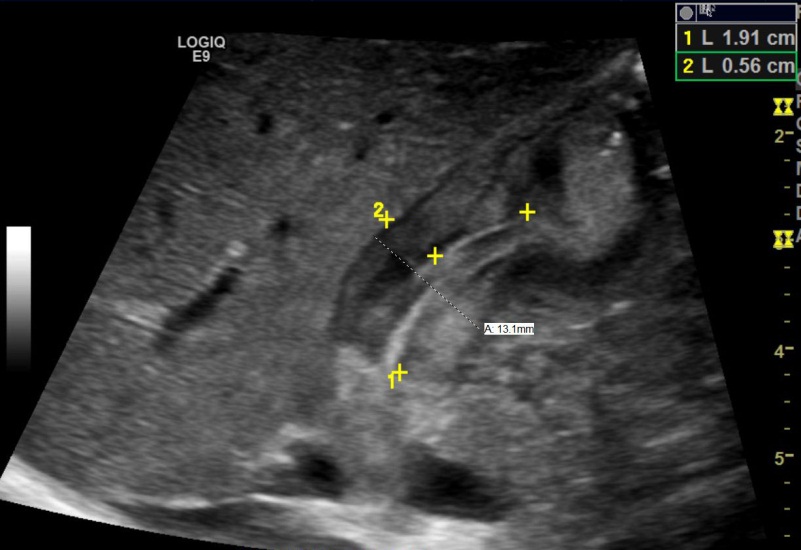
Treatment
Treatment is surgical with laparoscopic pyloromyotomy. Surgical consultation should be obtained once the diagnosis is made; however the surgery is not emergent and the patient should be well hydrated and any electrolyte abnormality should be corrected prior to surgery. Initial fluid resuscitation should be with normal saline boluses. Once the infant is well hydrated and the child is urinating, potassium chloride should be added to maintenance fluids.
Pearls and Pitfalls
- Pyloric stenosis should be considered in infants 3-6 weeks presenting with “projectile” nonbilious emesis.
- The classic metabolic derangement in HPS is a hypokalemic, hypochloremic metabolic alkalosis.
- When interpreting an ultrasound for pyloric stenosis, remember “pi= 3.14”. Measurements greater than 3 mm thickness and 14 mm length are consistent with HPS.
- Infants with pyloric stenosis do NOT present with bilious emesis. In infants with bilious emesis, other causes of vomiting such as malrotation with volvulus need to be considered.
References
- Ranells JD, Carver JD, and Kirby RS. Infantile hypertrophic pyloric stenosis: epidemiology, genetics and clinical update. Adv Pediatr 2011;58:195-206.
- Glatstein M, Carbell G, Boddu SK, et al. The changing clinical presentation of hypertrophic pyloric stenosis: the experience of a large, tertiary care pediatric hospital. Clin Pediatr 2011;50(3):192-195.
