- Describe pediatric bony anatomy
- Identify a Torus or Buckle fracture and describe its clinical significance
- List the different classifications of Salter Harris Fractures I-V
- Describe the clinical significance and treatment options for Salter Harris Fractures
Pediatric bony anatomy
The immaturity of the pediatric skeletal system often lends itself to significant differences with respect to orthopedic injuries. Subtle radiographic findings can be associated with fractures, and misinterpretation of a radiograph can lead to a lifelong functional deficits.
There are two anatomic considerations for the pediatric bone. First, the growing bone is less ossified and subsequently has a higher degree of plasticity. This plasticity makes results in unique fracture patterns not seen in adults, such as “torus or buckle” fractures and “greenstick” fractures. The second is the presence of the growth plate, or physis. The physis is a hyaline cartilage plate where bone growth primarily occurs. Proximal to the physis is the metaphysis. The epiphysis is located distal to the physis.
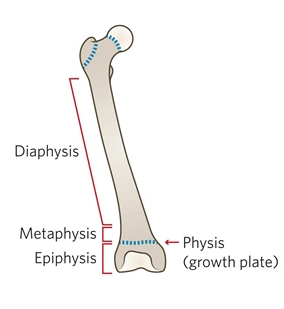
The position of a fracture relative to the metaphaphysis, physis, and epiphysis has a tremendous impact on the clinical significance of the fracture. Growth plate injuries are characterized by the Salter Harris classification system.
Initial Actions and Primary Survey
Clinical Presentation
There is a wide variety clinical presentations that are associated with pediatric orthopedic injuries. The most common mechanisms are axial load injuries and inversion/eversion injuries of the extremities. The mechanism of injury is an important part of the history to guide understanding of the potential injuries. It is important to rule out any other life-threatening injuries, but often children have focal pain that will guide the history, examination and evaluation of the child.
Physical exam findings are variable. Most children are reluctant to use the injured extremity and complain of significant pain with palpation. Localized swelling and deformity is typically also present. Check distal neurovascular status to ensure there is not limb-threatening injury before pursuing the orthopedic cause of the pain.
Diagnostic Testing
Plain film radiographs are typically sufficient to make a diagnosis. Localization of the injury may be challenging clinically so it is common for the joint above and below the suspected area of injury to be imaged as well.
CTs are not indicated for diagnosis of most pediatric fractures in the emergency department.
Differential Diagnosis – Fracture Types
Torus or Buckle Fracture
This type of fracture is characterized radiographically by a small bulging of the cortex. It most commonly occurs after an axial load injury. The most common location is at the junction of the dense bone of the diaphysis and more porous, immature bone of the metaphysis.
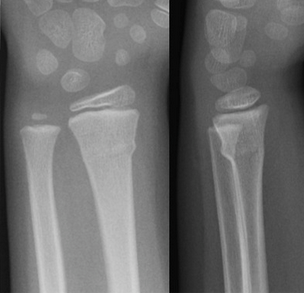
Treatment consists of splinting in the ER to prevent further injury and orthopedic follow up. No reduction is necessary. Immobilization is typically for less than one month.
Salter Harris Fractures
The Salter Harris classification system describes fractures that involve the growth plate, or epiphyseal plate. The distinctions between the different types are significant as it impacts treatment and prognosis of the injury. The SALTER mnemonic is useful for remembering the different classifications.
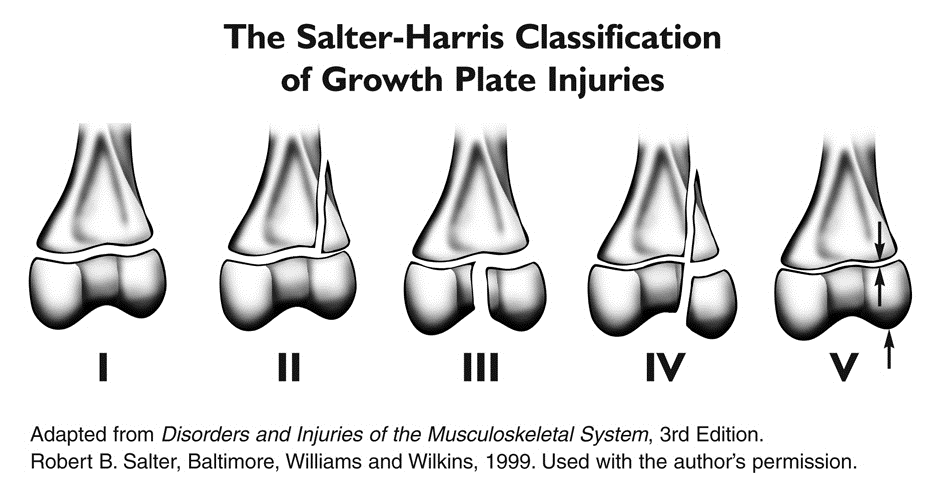
Salter Harris Type I
A Salter Harris Type 1 fracture goes directly through the physis and represents six percent of Salter Harris fractures. Often, there is no radiographic abnormality seen at the time of the fracture. If this is the case and the patient has pain overlying the physis, it is best to splint the joint and have the patient follow up with an orthopedist in one week for repeat imaging. The prognosis is good, and surgery is typically not indicated. If there is displacement of the epiphysis, urgent reduction will be needed.
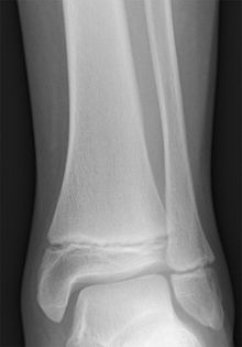
Salter Harris I, no Displacement noted
Salter Harris Type II
A Salter Harris Type II fracture travels through the physis and then travels proximally through the metaphysis. This is the most common Salter Harris Fracture, accounting for 75% of all growth plate injuries. This most commonly occurs after the age of 10 and often does not require surgery or result in a significant long-term functional limitation and good prognosis. Fractures with angulation and displacement may need reduction. Acceptable amounts of angulation will vary depending on the age of the patient and location of the fracture.
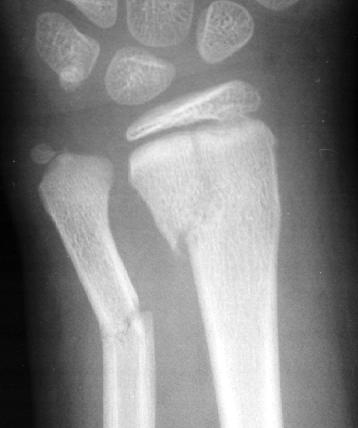
Salter Harris II of the distal radius with associated Ulnar Fracture
Salter Harris Type III
A Salter Harris Type III fracture travels through the physis and then distally through the epiphysis into the joint space, making it an intra-articular fracture. This accounts for 7-10% of growth plate injuries and also typically occurs after the age of 10. The prognosis is often poorer as the proliferative and reserve zones of the growth plate are interrupted. Early reduction is crucial to long term outcomes and orthopedics should be consulted in the ER for all displaced fractures. Surgical treatment is often needed to achieve proper reduction and preservation of growth plate integrity. Non-displaced fractures should be splinted and expeditious orthopedics follow up should be arranged.
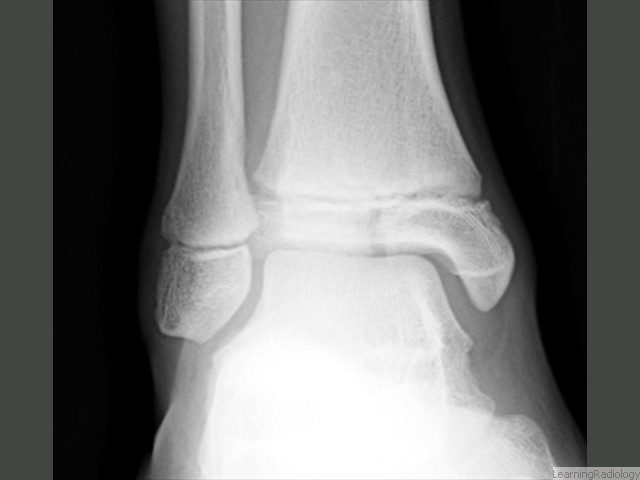
Salter Harris III of distal tibia
Salter Harris Type IV
A Salter Harris IV fracture travels from the metaphasis, through the physis, and finally through the epiphysis and into the joint space, making it an intra-articular fracture. This accounts for roughly 10% of all growth plate injuries and typically carries a poorer prognosis. Once again, early reduction is crucial and orthopedics should be consulted in the ER for all displaced Salter Harris IV fractures, as surgical treatment is often necessary. Orthopedics should be called for all non-displaced fractures to ensure expeditious follow up.
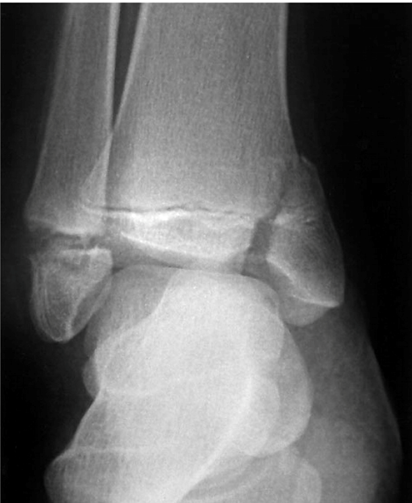
Salter Harris IV of distal tibia
Salter Harris V
A Salter Harris V fracture involves an axial loading mechanism with compression of the physis. This is relatively rare and accounts for less than one percent of growth plate injuries. Proper diagnosis is dependent upon recognition of a mechanism of a significant axial load force on the extremity. Radiographic changes are subtle, and involve narrowing of the physis with a joint effusion. Misdiagnosis is common and prognosis is poor, being associated with significant growth disruption. There is typically not significant displacement present, but orthopedics should be consulted to arrange follow up in anticipation of growth arrest.
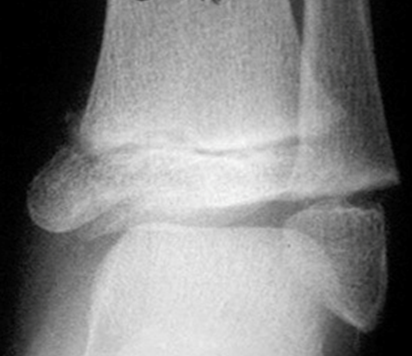
Salter Harris V of distal tibia
Disposition
The vast majority of pediatric fracture patients will be discharged home. Exceptions include significantly displaced fractures that require operative treatment. It is important to provide adequate analgesia both in the ER and at home.
Pearls and Pitfalls
- Have a high index of suspicion for fracture with any child that has an acute functional limitation in an extremity.
- Imaging of joint above and below apparent injury is crucial to ensure that no fractures are missed.
- “Normal” imaging does not exclude a fracture.
- It is perfectly acceptable to splint a patient and have them follow up for repeat imaging if the child has persistent pain or a functional limitation.
- Always document neurovascular status before and after splint placement.
References
- http://www.hawaii.edu/medicine/pediatrics/pemxray/v3c05.html
- http://rad.usuhs.edu/medpix/kiosk_image.html?imageid=21433&quiz=#pic
- Menkes, J.S. Orthopedic Injuries. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide Chapter 267
- http://emedicine.medscape.com/article/412956-overview
- Up to Date Salter Harris Classification of Physeal Fractures
- http://www.rch.org.au/fracture-education/anatomy/Anatomic_differences_child_vs_adult/
- Wheele’s textbook of Orthopedics, Salter Harris Fractures
- http://radiopaedia.org/articles/salter-harris-fractures
