Pneumonia
Home
/
About SAEM
/
Academies, Interest Groups, & Affiliates
/
CDEM
/
For Students
/
CDEM Curriculum
/
M4 Curriculum
/
Pneumonia
Author: Olivia Bailey, Associate Professor of Emergency Medicine, University of Iowa
Aaron Hultgren,Liliya Abrukin NYU School of Medicine and Bellevue Hospital Center
Editor: Alisa Hayes, Associate Professor of Clinical Emergency Medicine, University of Missouri - Columbia
Last updated: 2019.
Case Study
An 82-year-old male is brought in by his granddaughter from home for fever and productive cough that started earlier in the day. He has a past medical history of congestive heart failure and coronary artery disease. His vitals include a of temperature 38.5°C, heart rate of 110, blood pressure of 128/61, and an oxygen saturation of 92% on room air. You hear rales and rhonchi in the right mid-lung. How will you evaluate, treat, and disposition the patient?
Objectives
Upon finishing this module, the student will be able to:
- Identify the common pathogens in pneumonia.
- Discuss diagnostic considerations for evaluating pneumonia.
- Describe the management and antibiotic treatment for pneumonia.
- Discuss discuss the disposition of patients with pneumonia.
Introduction
Pneumonia is a common infection and causes significant morbidity and mortality in the United States. In the US, it is the 8th leading cause of death, the most common cause of death from infection, and the 2nd most common cause of hospitalization in the United States. Physicians in the emergency department need to be able to diagnosis, appropriately treat, and disposition patients with pneumonia.
It is important to understand the different classifications of pneumonia.
Community-acquired pneumonia (CAP) is lung parenchyma infection in a non-hospitalized patient.
Hospital-acquired pneumonia (HAP) or nosocomial pneumonia is a new lung parenchyma infection that occurs after 48 hours of hospitalization.
Ventilator-associated pneumonia (VAP) occurs in the subset of HAP patients that are mechanically ventilated.
Healthcare-associated pneumonia (HCAP) is no longer a classification that is utilized. Given the patient population of emergency medicine, the focus of this chapter will be on CAP.
Historically, pathogens have been divided into “typical” and “atypical.” Typical pathogens include Streptococcus pneumoniae (most common), Haemophilus influenzae, Staphylococcus aureus, Group A streptococci, Moraxella catarrhalis. Atypical pathogens include Mycoplasma pneumoniae, Chlamydophila pneumonia, Legionella species. Viruses such as influenza, parainfluenza, and respiratory syncytial virus can also cause pneumonia as can fungi.
Risk factors for pneumonia include increased age, chronic comorbidities such as COPD, viral upper respiratory infections, smoking, heavy alcohol use, difficulty protecting the airway or other lifestyle factors such as crowded living conditions.
Signs and Symptoms
Patients with pneumonia may present with signs and symptoms such as fever, chills, cough, pleuritic pain, sputum production, chest pain, shortness of breath, anorexia or malaise. Elderly patients may present with fatigue, confusion or delirium. There can be a range of vital sign abnormalities depending on severity, including tachypnea, tachycardia, hypoxia and hypotension. Patients may present in septic shock as a result of pneumonia.
Initial Actions and Primary Survey
All patients should have a set of vital signs including temperature, pulse, blood pressure, pulse oximetry, and respiratory rate. The “ABCs” approach focuses on stabilizing airway, breathing, and circulation. Acutely ill patients will need peripheral access, monitoring, and supplemental oxygen, as well as early antibiotics and pressors if the present in septic shock. Patients in respiratory distress may require supplemental oxygen, noninvasive positive pressure ventilation, or endotracheal intubation.
ABCs
Airway - Evaluate the airway for stridor, edema, or upper airway obstruction.
- Actions:
- Reposition patient airway.
- Place patient on nasal cannula and/or a non-rebreather. (use both for preoxygenation if preparing to intubate).
- Perform airway maneuvers/adjuncts such as head tilt/chin lift, jaw thrust, or nasal trumpet insertion.
Breathing – Assess for adequate ventilation. Look for tachypnea, increased work of breathing, and signs of respiratory distress such as nasal flaring, retractions, or tripoding. Imminent or impending respiratory failure may require endotracheal intubation with rapid sequence intubation (RSI).
- Actions may include:
- Supplemental oxygen (nasal cannula or non-breather)
- Non-invasive ventilations (BIPAP)
- Invasive ventilation (with rapid sequence endotracheal intubation)
Circulation – Assess perfusion of vital organs and identify signs of cardiovascular compromise from pneumonia causing sepsis or septic shock.
- Actions may include:
- Place 2 large-bore peripheral IVs
- Saline bolus of 30cc/kg
- Early broad-spectrum antibiotics
- Severe sepsis and septic shock patients may require central line placement and vasopressor support.
Disability – Assess patient’s mental status. Pneumonia may cause respiratory compromise resulting in hypoxia, hypercarbia, or respiratory failure leading to somnolence, confusion, and altered mental status. Poor mentation and inadequate protection of the airway may require intubation. Patients who cannot protect their airway should not be placed on non-invasive ventilation. Consider aspiration pneumonia in patients with decreased mental status or conditions that may lead to dysphagia.
Presentation
Classically the “typical” CAP caused by Streptococcus pneumoniae is described as presenting with the sudden onset of fever, productive cough, and pleuritic chest pain. Atypical CAP may have a more protracted course beginning with upper respiratory symptoms, slowly worsening cough, malaise and fatigue. These classic presentations of typical and atypical pneumonias are not considered to be sensitive or specific for identifying pneumonia in prospective studies.
“Classic” Presentations:
Typical Pneumonias
- Streptococcus pneumoniae – bloody or rust-colored sputum, single episode of shaking chills
- Haemophilus influenzae – fever, muscle pain, fatigue, history of COPD, smoker
- Klebsiella pneumoniae – currant jelly sputum, bulging minor fissure, often right upper lobe. Alcoholics, diabetics, and COPD patients are at risk.
Atypical Pneumonias
- Mycoplasma pneumoniae – “walking pneumonia;” upper respiratory symptoms, gradually worsening over weeks or even months, bullous myringitis may be present
- Chlamydophila pneumoniae – pharyngitis, laryngitis and sinusitis, associated with outbreaks in close-contact settings (dorms, prisons), staccato cough
- Legionella – respiratory and gastrointestinal symptoms, relative bradycardia
- Pseudomonas aeruginosa risks factors: immunocompromised, cystic fibrosis
Aspiration Pneumonia
- This occurs when there is aspiration of colonized oropharyngeal material. It should be differentiated from aspiration pneumonitis which is a chemical injury from inhalation of gastric contents due to regurgitation that can occur with drug overdose, seizures, cerebrovascular accident, or use of anesthesia. Patients at risk for aspiration include patients with dysphagia due to neurologic disorder, nursing home residents, and patients who abuse alcohol.
- Immunocompromised Patients represent a special subset of pneumonia given the increased susceptibility to a spectrum of potential pathogens. Patients comprising this population include those with solid organ transplants, cystic fibrosis, HIV/AIDS, hematopoietic cell transplants, pregnant women, and patients with other immune defects.
- General considerations include obtaining a thorough past medical history, as well as asking about medications such as chemotherapy, immunomodulating agents, and chronic steroid use. Leukopenia and CD4 count may guide evaluation and treatment considerations.
- Pneumocystis jirovecii (previously classified as Pneumocystis carinii) is typically found in immunocompromised patients, such as those with HIV/AIDS. Symptoms include dyspnea, nonproductive cough, and fever. Chest x-ray usually shows bilateral infiltrates, but may also present with lobar consolidation. Treatment is trimethoprim-sulfamethoxazole (TMP-SMX) and adjunctive corticosteroids in severe disease.
- Tuberculosis is another important consideration in immunocompromised patients as well as patients with a history of prior tuberculosis infection, night sweats, weight loss, or exposure from shelters, prisons, or recent travel to endemic areas.
Physical Examination
A full physical exam is important to both evaluate for alternative diagnoses as well as clues related to a particular pneumonia. The physical exam starts with initial vitals and inspection of the patient for respiratory distress. Patients sitting upright or in the “tripod position” with nasal flaring, chest retractions, and abdominal breathing exhibit an increased work of breathing and may have impending respiratory failure. Review of vital signs may show tachypnea, tachycardia, hypotension, hypoxia, and fever. Examination of the chest involves a four-step process: inspection, palpation, percussion, and auscultation of the chest. The positive predictive value of abnormal breath sounds in acute respiratory illness is 55%, further illustrating the difficulty in diagnosing pneumonia with the physical exam. There are no individual or combination of clinical findings that rule in the diagnosis of pneumonia (Metlay et al. 1999).
Examiners should look for other causes of dyspnea with their associated presentations, such as congestive heart failure, pericardial effusions, pleural effusions, pulmonary embolus, and neoplasms. Lastly it is important to evaluate the head, ears, eyes, nose, and throat as many of these patients may initially had an upper respiratory infection that developed into a bacterial pneumonia and concomitant bacterial infections.
Diagnostic Testing
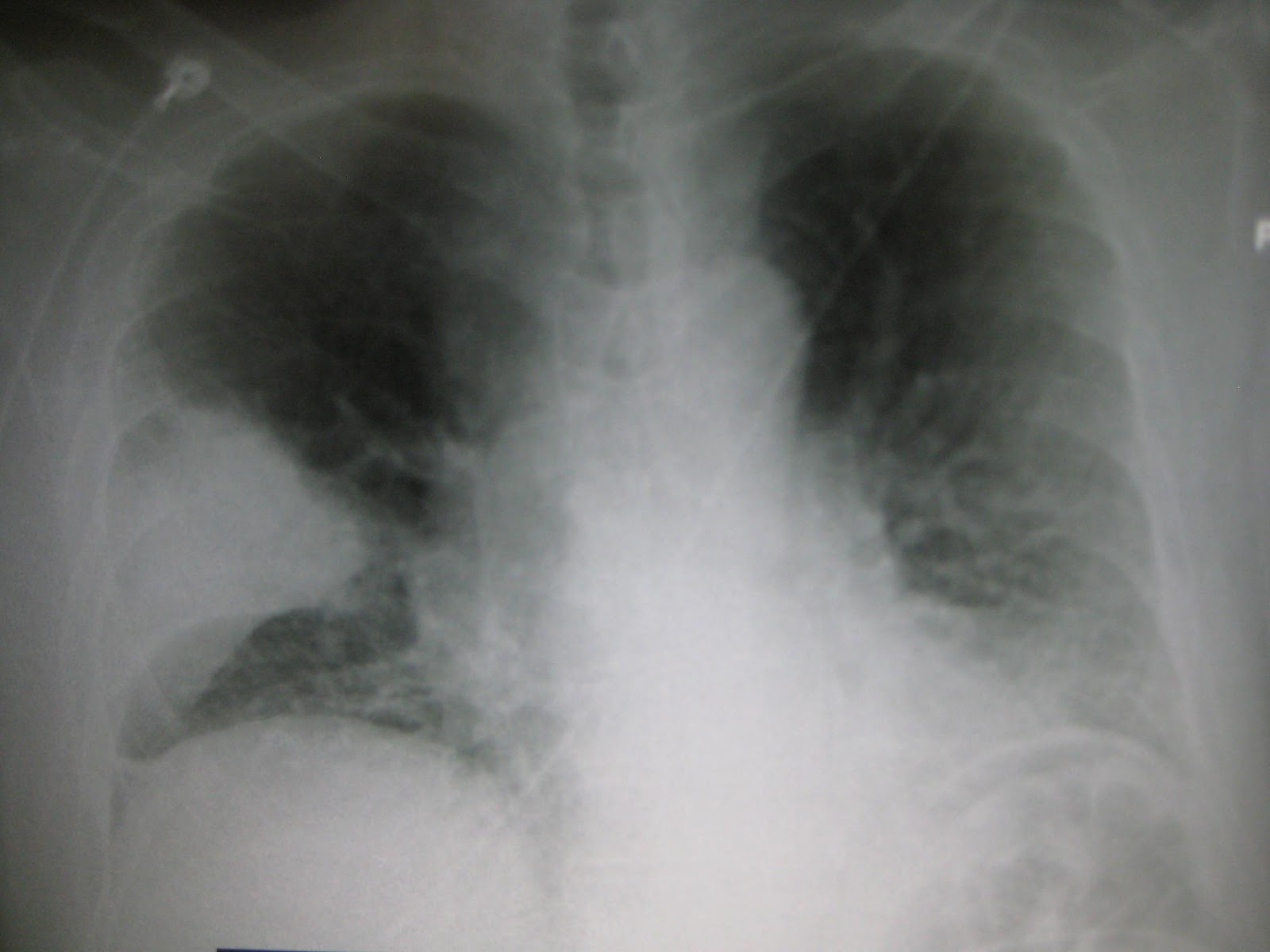
Figure 1 (Above): Right middle lobe pneumonia on chest x-ray. Image Used with Permission by James Heilman, MD
Chest radiography is the main diagnostic modality to evaluate for pneumonia in the ED setting, although it is not always confirmatory. Absence of abnormal vital signs or abnormalities on chest examination reduces the likelihood of pneumonia and the need for further diagnostic studies (Metlay et al. 1999). Factors that predict pneumonia on chest x-ray include temperature >37.8 OC, tachycardia, absence of asthma, rales, and locally decreased breath sounds on auscultation. Pulmonary infiltrates on chest x-ray confirm the clinical diagnosis.
Lobar consolidation is typical of Streptococcus pneumoniae or Klebsiella pneumoniae while multi-lobar infiltrates are more consistent with Staphylococcus aureus and Pseudomonas aeruginosa. Atypical infections such as Mycoplasma pneumoniae, Chlamydophila, and Legionella may reveal patchy infiltrates on radiography. Despite these patterns on chest radiography, it is important to note that typical pathogens can present with diffuse infiltrates and atypical pathogens with discrete consolidations. Radiographic evidence of pneumonia may not be evident on initial chest radiography in patients with early aspiration pneumonias or severe dehydration; however, infiltrates may present on later imaging. Posteroanterior and lateral chest radiographs are recommended in patients that are able to stand and are stable enough to travel to radiology.
Bedside ultrasound is a reliable, noninvasive diagnostic tool for the detection of pneumonia in children, adolescents and adults, with a sensitivity of 86%, a specificity of 89% and a LR 7.8 (95% CI, 5.0-12.4) (Shah et al. 2013). Emergency physicians with advanced sonography skills may be able to identify consolidation. However, ultrasound is operator dependent and therefore its use is only as good as its user. Ultrasound can be very useful in identifying or guiding drainage of pleural effusions related to pneumonia.
Computer Tomography of the chest is more sensitive than plain films of the chest and may be used with patients with an equivocal chest x-ray or when other etiologies for the patient’s presentation are suspected such as pulmonary embolism or mass.
An EKG should be ordered on patients with pneumonia, especially those with tachycardia, chest pain, hypotension or who are ill appearing. Patients with congestive heart failure, cardiovascular disease, and severe sepsis/septic shock may develop cardiac ischemia and infarction secondary to a severe pneumonia.
Blood cultures should be obtained in any patient ill enough to require ICU admission or mechanical ventilation, all patients with suspected sepsis, as well patients with CAP that are at increased risk for bacteremia and resistant organisms.
These risk factors for CAP patients include:
- Cavitary lesions
- Leukopenia
- Chronic severe liver disease
- Asplenia
- Pleural effusion
- Alcohol abuse
- Severe CAP
Sputum induction for gram stain and culture should not be routinely performed in the emergency department as it poses an infection risk to both providers and other patients and is unlikely to change ED management.
Treatment
Antimicrobial treatment options for pneumonia may change depending on a number of factors, including local sensitivities and institutional availability. Refer to institutional antimicrobial stewardship guidelines for determining antibiotic regimens.
Outpatient Treatment:
- Previously healthy and no antibiotics in past 3 months
- Macrolide or doxycycline
- Comorbidities like chronic heart, lung, liver, or renal disease, diabetes, alcoholism, immunosuppression, cancer, asplenia or antibiotics in past 3 months
- Respiratory fluoroquinolone OR
- Beta-lactam PLUS a macrolide
Inpatient, non-ICU Treatment:
- Respiratory fluoroquinolone OR
- Anti-pneumococcal beta-lactam PLUS a macrolide
Inpatient, ICU Treatment:
- Anti-pneumococcal beta-lactam PLUS azithromycin OR
- Anti-pneumococcal beta-lactam PLUS respiratory fluoroquinolone OR
- For penicillin-allergic patients, respiratory fluoroquinolone PLUS aztreonam
If Pseudomonas aeruginosa is a consideration:
- Piperacillin-tazobactam, cefepime, imipenem, or meropenem PLUS ciprofloxacin or levofloxacin
If community-acquired MRSA is a consideration (empyema, recent influenza, IV drug use, abscess, severe pneumonia):
- Add vancomycin or linezolid
Table 1: Antibiotics for Treatment of Pneumonia
Aspiration Pneumonia:
- Ampicillin-sulbactam or amoxicillin-clavulanate
- If poor dentition: imipenem, meropenem, or piperacillin-tazobactam
Disposition
Clinical judgment is essential to determine the disposition of the patient with CAP as patients may be treated as an outpatient, placed in an observation unit, or treated as an inpatient on a floor or ICU. Patients with the inability to tolerate oral antibiotic treatment, hypoxia, sepsis, or respiratory distress will require admission. Patients with pneumonia with severe sepsis or septic shock will need critical care management. Risk stratification instruments may aid emergency clinicians on patient disposition for community-acquired pneumonia. Review the prediction rules listed below via the links.
Pneumonia Severity Index (PSI): https://www.mdcalc.com/psi-port-score-pneumonia-severity-index-cap
CURB-65: https://www.mdcalc.com/curb-65-score-pneumonia-severity
Pearls and Pitfalls
- Management of pneumonia should start with an ABC approach and stabilization of the patient with an acute pneumonia.
- Identify appropriate antibiotics. Familiarize yourself with your local antibiogram and institutional stewardship guidelines.
- Chest radiography continues to be the mainstay for diagnosis of pneumonia; however, ultrasound and CT scan may be helpful in certain situations.
- Disposition of patients with pneumonia should be based on clinical judgment along with risk stratification instruments.
- Patients with a new oxygen requirement or who are unable to take oral antibiotics will generally require admission.
Case Study Resolution
Your patient’s oxygen saturation improved with 2L oxygen via nasal cannula. An IV fluid bolus is ordered. Chest X-ray confirms pneumonia. Treatment with ceftriaxone and azithromycin is started. You suspect the patient would benefit from hospitalization, and this is supported by the PSI score you calculated. Patient is admitted to the floor for further care.
References
Corbo J, Friedman B, Bijur P, Gallagher EJ. Limited usefulness of initial blood cultures in community acquired pneumonia. Emerg Med J. 2004; Jul;21(4):446-448. PMID: 15208227
Fine MJ, Auble TE, Yealy DM, et al. A prediction rule to identify low-risk patients with community acquired pneumonia. N Engl Med. 1997; 336: 243-250. PMID: 8995086
Halm EA, Teirstein AS. Clinical Practice. Management of community-acquired pneumonia. N Engl J Med. 2002 Dec 19;347(25): 2039-2045. PMID: 12490686
Mandell LA, Wunderink RG, Anzueto A, et al. Infectious Disease Society of America/American Thoracic Society consensus guidelines on the management of community-acquired pneumonia in adults. Clin Infect Dis 2007; 44 Suppl 2:S27. PMID: 17278083
Marik PE. Aspiration Pneumonitis and Aspiration Pneumonia. N Engl J Med. 2001; 344: 665-671. PMID: 11228282
Metlay JP, Kappor WN, Fine MJ. Does this patient have community-acquired pneumonia? Diagnosing pneumonia by history and physical examination. JAMA 1997: 278(17): 1440-1445. PMID: 9356004
Plouffe JF, Martin DR. Pneumonia in the emergency department. Emergency medicine Clinics of North America. 2008 May;26(2):389-411. PMID: 18406980
Slaven EM, Santanilla JI, DeBlieux PM. Healthcare-associated pneumonia in the emergency department. Semin Respir Crit Care Med. 2009 Feb;30(1):46-51. PMID: 19199186
