Lumbar puncture
Author Credentials
Author: Julia Dixon MD, University of Colorado School of Medicine, David Richards MD, Denver Health Emergency Medicine, and Kaitlin Roth MD, Denver Health Emergency Medicine
Update Editor: Doug Franzen, MD, M.Ed
Section Editor: William Alley, MD
Last updated: 2023
Case Study
A 68 year old female, Mrs. A, is brought in by ambulance after being found down in her home by her son one hour prior to arrival. Son reports his mother lives alone and was in her normal state of health until yesterday when she began complaining of a headache. Today he found her lying on the floor of her apartment and promptly called 911. Her vitals en route were: T 38.6 HR 96 BP 110/87 RR 14 SpO2 96% . On your initial exam, the patient is breathing spontaneously, GCS 7 withdraws all four extremities to pain, groans intermittently, and does not open her eyes to pain, no signs of trauma.
Objectives
By the end of this module, the student will be able to:
- List the indications for lumbar puncture
- Recognize the common presentations of illnesses requiring lumbar puncture
- Explain the risks and benefits of lumbar puncture as discussed when obtaining informed consent
- Describe the lumbar puncture procedure technique
- Order and interpret CSF lab studies
- List complications of lumbar puncture
- Recognize special considerations in select patient populations
Introduction
Lumbar puncture is a common emergency department procedure that is used for both diagnostic and therapeutic purposes. As a diagnostic tool, lumbar puncture is used to detect CNS infections, CNS malignancies, and inflammatory processes, such as Multiple Sclerosis or Guillain-Barre. Lumbar puncture also has historically been used in the diagnosis of subarachnoid hemorrhage (SAH) as the next diagnostic step in patients whose initial CT head is negative. However, this topic has become controversial and will be discussed in more detail below. Lumbar puncture is also used as a therapeutic and diagnostic tool in patients with idiopathic intracranial hypertension (IIH, or pseudotumor cerebri). Initial opening pressures should be performed on all patients and will help guide clinicians in diagnosis. CSF samples should be sent for cell count, gram stain, culture, glucose, protein, and in some cases specific viral and antibody serologies or flow cytometry to help guide clinical decision-making.
Before performing a lumbar puncture, providers must be well versed in different approaches to the procedure and be aware of potential complications. As with any procedure, good preparation is key to a successful outcome.
Initial Actions and Primary Survey
Primary Survey
In patients who present with significant altered mental status, it is important to quickly perform a primary survey to assess the patient’s airway, breathing, and circulation. There should be a particular focus on obtaining accurate Glasgow Coma Scale (GCS) and performing a thorough neurologic exam. Patients with a GCS score of less than 8 will require an advanced airway. Patients presenting in status epilepticus may require heavy sedation to stop seizing, which should also prompt providers to prepare for intubation. Altered patients must be undressed completely and the provider should perform an examination from head to toe. Look for any signs of trauma, bruising or lacerations on the body. Don’t forget to roll the patient to examine the back. A rectal tone should be assessed if the patient is unresponsive. Are there any rashes, transdermal drug patches, or medical bracelets on the patient? Check a core temperature and a blood sugar. Gather additional history from EMS, such as how was the patient found and what did the scene look like? How warm was the room? In order to obtain further history, call family or caregivers.
Initial Actions - Thinking back to the case, what work-up and treatment would you do for Mrs. A?
Initial work-up would include include basic labs (CBC, BMP, LFTs), lactate, blood cultures, urinalysis, urine drug screen, ethanol levels, VBG, ECG, chest-x ray, CT- Head and Neck (additional imaging may be done based off initial work-up). Empiric antibiotics should be started promptly if providers have high suspicion for meningitis. Antibiotics should not be delayed prior to obtaining the lumbar puncture. Prompt antibiotic administration within 2 hours of arrival decreases in-hospital mortality risk. Antibiotic resistance and sensitivities vary from hospital to hospital. For most places, Mrs. A should be empirically started on ceftriaxone, vancomycin, ampicillin. Some facilities may recommend starting empiric steroids, but this topic is controversial and may not be typical practice everywhere. Antibiotic selection should be narrowed when culture data is available.
Presentation
The presentation of disease states that require Emergency Department lumbar puncture vary widely. We will touch on the most common ED indications for lumbar puncture. Chief complaints when lumbar puncture should be considered include severe headache (particularly when combined with fever, nausea, or photophobia), altered mental status, weakness, and seizures.
Meningitis
Bacterial meningitis is classically taught as the triad of fever, neck stiffness, and altered mental status, but this triad is present in less than half of patients with the disease. One study from NEJM found that the most common presenting symptoms are severe headache and fever, found in 84% of patients and 77% of patients respectively. The study concluded that 95% of patients with bacterial meningitis presented with at least two of the following four symptoms: headache, fever, neck stiffness, and altered mental status. In other words, the classic triad plus headache. Viral and fungal causes of meningitis present similarly to bacterial meningitis, but the onset is usually more subacute and symptoms may be more subtle.
Subarachnoid hemorrhage
Subarachnoid hemorrhage (SAH) presents as a sudden onset headache < 1 hour to maximum severity, and can be described as “the worst headache of my life.” Other symptoms include loss of consciousness, stiff neck, nausea, and vomiting. Patients with these symptoms must be sent for a CT head without contrast to evaluate for blood. According to some studies, the sensitivity for SAH with a modern CT scanner and skilled radiologist is as high as 93%, which increases if performed within 6 hours of headache onset*. In CT negative patients where clinical suspicion is high for SAH, a lumbar puncture to evaluate for xanthochromia can be done. It is important to note that traumatic taps can introduce blood into CSF due to the procedure itself, which can complicate the interpretation of CSF studies. With such controversial data and ideas, it is important to have a shared decision-making conversation with the patient regarding the risks of performing and not performing a lumbar puncture in diagnosis of SAH.
Multiple Sclerosis
Multiple Sclerosis (MS) is a difficult diagnosis to make due to its relapsing and remitting nature and wide variety of presentations. Patients may present with sensory loss in limbs, painful monocular vision loss, diplopia, ataxia or balance issues, dysarthria, urge incontinence, or Lhermitte sign (electric shocks that travel down the spine with neck flexion). CSF samples are not always required to make the diagnosis of MS. Patients with MRI studies suggestive of lesions disseminated in both space and time will not need a confirmatory lumbar puncture. However, in patients who have MRI findings that are less diagnostic, a lumbar puncture is the next step. CSF samples will show oligoclonal bands in up to 95% of patients with MS.
Guillain-Barre Syndrome
Guillain-Barre Syndrome (GBS) may present with symmetrical limb weakness initially in the legs (can also present initially in the arms or facial muscles), paresthesias in the hands or feet, diminished deep tendon reflexes, fever, tachycardia, hyper/hypotension, urinary retention or ileus.
Idiopathic Intracranial Hypertension
Idiopathic Intracranial Hypertension (IIH), also known as pseudotumor cerbrebri, is associated with obesity and affects females more than males. Patients will commonly present with headache and changes in vision, such as visual obscurations that change with position, flashes of light, vision loss, or diplopia. The hallmark physical exam finding is papilledema. Patients with suspected IIH must obtain neuroimaging prior to receiving a lumbar puncture to exclude other secondary causes of increased intracranial pressures (ICP), such as intracranial masses or venous sinus thrombosis. Preferred neuroimaging includes both MRI with and without contrast and magnetic resonance venography (MRV). MRV helps to evaluate for venous sinus thrombosis. During the lumbar puncture, patients need to lie on their side to obtain accurate opening pressures. An opening pressure of >25 cm H2O, along with papilledema and typical clinical story will be diagnostic of IIH. Therapeutic use of lumbar puncture in IIH is controversial as CSF typically reaccumulates quickly. In patients whose symptoms are severe and recur quickly, definitive surgery may be necessary to prevent vision loss.
There are other diseases where lumbar puncture is part of the diagnostic work up including, autoimmune encephalitis, CNS malignancies, CNS vasculitis, and paraneoplastic syndromes which are not discussed here.
The evaluation of CSF will help you determine the diagnosis. Specific CSF analyses are illustrated in the lab studies section.
Diagnostic Testing
Indications for lumbar puncture
- Signs and symptoms concerning for meningitis (ie fever, headache, neck stiffness)
- Altered mental status without other clear etiology
- Focal neurologic deficits with negative stroke work-up (to evaluate for conditions like Multiple Sclerosis or Guillain-Barre syndrome)
- Evaluation for CT negative Subarachnoid Hemorrhage
- Signs and symptoms of Idiopathic Intracranial Hypertension
Contraindications
Coagulopathy (including oral anticoagulants)
Thrombocytopenia (typically platelets less than 20,000 warrant transfusion before the procedure)
Known intracranial process causing mass effect
Cellulitis or abscess of skin over the procedure site
Suspected spinal epidural abscess
Obtaining informed consent
Informed consent should be obtained in the patient’s primary language. If a patient is confused or altered, obtain informed consent from a family member or designated medical decision-maker. The provider should use simple terms understandable
to the patient and clearly explain why the procedure is indicated and describe the procedure. The risks of the procedure include post lumbar puncture headache (10-30%), epidural hematoma, subdural hematoma, damage to nerves, paraparesis, subtonsilar
herniation (<1%), radicular symptoms, epidermoid tumor, persistent CSF leak and a dry tap. Explain to the patient or medical decision-maker that significant complications are very rare and clarify the benefits of the procedure, as well as list
alternatives.
Procedure technique
A good video of performing a lumbar puncture can be found in the New England Journal Of Medicine’s collection of procedural videos. This video will help understand the following sections.
Gathering supplies and setting up the room
The first step is to gather supplies, (Table 1). Many facilities stock premade kits containing most supplies except sterile gloves. It is always good to have an extra needle and additional local anesthetic.
Once you have gathered your supplies, make sure that the room is set up in a way that is most convenient for you. Raise the bed to a comfortable height so that you are not hunched over. Place your supplies on a clean stand with plenty of space. Bring a trash can nearby to make clean up easier.
Table 1: Supplies needed for Lumbar Puncture
| Sterile Gloves | Collection Tubes (4) |
| Mask | Monometer with 3 way valve |
| Betadine or chlorhexadine | 5cc Syringe |
| Local anesthesia-Lidocaine 1or 2% | 18G or blunt needle |
| Sterile Drape or Towel | 25G or 27G needle |
| Spinal Needle *** | Systemic analgesia |
*Ideally 20G or 22G – large diameter needles are associated with increased risk of post lumbar puncture headache and persistent CSF leak. Spinal needles come in different lengths and are specifically made with occluding stylets to prevent the cutting effect of the needle tip as it penetrates the dura. Some have special tips (ex: Whitacre or Sprotte) thought to spread the dural fibers instead of cutting them.
2. Positioning
The next step is to position the patient. (fig 1) You may need to treat pain first to facilitate patient comfort and cooperation. Infants and young children will be in the lateral decubitus position, laying on the left or right side. Infants can be held by another person with care taken to ensure the patients respiratory status is not compromised by curling the infant too tight.
Adults and larger children are positioned on their side and asked to curl their back out like a cat arching, with their knees brought towards the chest and chin tucked down. Adjust the hips and shoulders perpendicular to the bed without any twisting of the spine. Adults can also have the procedure performed in the sitting position with their legs over the edge of the bed, back arched out and chin tucked, offering a pillow to hug can help keep patients in this position. This can make it easier to find landmarks in obese patients, but opening pressures cannot be accurately measured in sitting patients.
Good positioning and landmark identification is THE KEY to performing the procedure successfully.
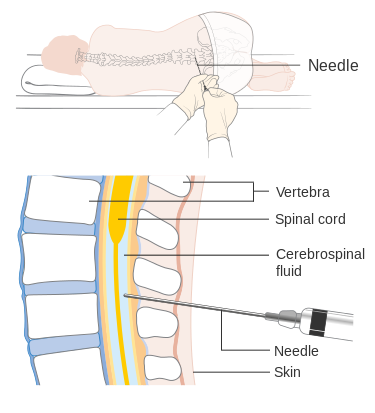
Figure 1: Top: Patient placed in left lateral decubitus with the knees curled upward and the chin tucked down toward the chest. The site of entry is at the L4-L5 interspace. Bottom: Sagittal view of the spinal column. The needle should pass between the spinous processes, through multiple layers of ligaments (supraspinous ligament, interspinous ligament, and ligamentum flavum) and end in the subarachnoid space. Attribution: Cancer Research UK / Wikimedia Commons
3. Identifying landmarks
To identify your landmarks palpate the anterior iliac crests, an imaginary line connecting the two iliac crests crosses the L4 spinous process. Palpate the spinous processes at the level of this line, carefully identifying midline. The spinal needle should be introduced at the L2-L3, L3-L4 or L4-L5 interspace. Mark the interspace at midline with a skin marker or by indenting the skin with the needle cap.
4. Aseptic technique
Once you’ve gathered all necessary supplies, optimized the room set-up for efficiency, positioned the patient properly, identified landmarks, and marked the skin, you can put on your sterile gloves. Prep and drape the patient using sterile technique. Clean at least a 10cm area with betadine or chlorhexidine scrub using a circular motion. If the kit comes with premade drapes, use the solid drape between the back and bed and position the opening in the fenestrated drape where you marked the skin. Sterile towels can also be used.
Palpate landmarks and reconfirm midline and the level you are going to insert the needle using sterile technique. At the marked site, provide local anesthesia using 1% or 2% lidocaine. Insert the local anesthesia needle in the same space, initially making a subcutaneous wheel and then directing the needle into the interspinous space to provide deeper anesthesia. Probing with the anesthesia needle can also help identify locations of spinous processes when they are difficult to palpate. Ultrasound can also be helpful in locating bony landmarks in morbidly obese patients
While the anesthetic is beginning to take effect, you should set up the lumbar puncture tray. Prepare your manometer, many manometers come as two pieces that need to be connected. Connect the manometer to the three way valve at the vertical position, the knob on the valve points to the port that is off. Remove the caps and position the collection tubes #1 through #4 in an order that you will remember.
5. Procedure technique
Reconfirm the site of needle insertion by palpating landmarks. Use the side of your non-dominant hand to brace against the patient’s back and stabilize the tip of the needle between your index finger and thumb. Use your dominant hand to apply pressure and advance the needle with the stylet in place. The bevel edge of the needle should be parallel to the ligament fibers that run head to toe. The bevel will be up when the patient is on their side and to the right or left when they are sitting upright. The needle will point slightly caudal, towards the patient’s umbilicus (see Fig 1).
Proceed through the skin, subcutaneous tissue, supraspinous ligament, interspinous ligament and finally the ligamentum flavum. It is often possible to feel a pop when going through the ligamentum flavum. Remove the stylet and look for flow of CSF. If no CSF is present, slowly advance the needle 1-2 mm at a time and remove the stylet and look for flow of CSF. If the needle hits bone superficially it likely has hit a spinous process and needs to be redirected rostral or caudal. If it contacts bone deeper, it has likely hit a transverse process, indicating the needle needs to be redirected in a medial/lateral direction. Be sure to retract the needle into the subcutaneous space without removing the tip from the patient and then redirect the angle before readvancing the needle
Once CSF is visualized, attach your manometer to the needle and allow the fluid to flow and measure the pressure. Of note, you must have your patient relax their legs, so as to not falsely elevate the pressures. Use one hand to stabilize the needle, slight variations occur with respiration. Normal pressure for adults is in the range of 7-18 cmH2O. Use the collection tubes to obtain approximately 1ml of fluid per tube. (Fig 2)

Figure 2: CSF in Vials. Image courtesy of James Heilman, MD. This image is used under the Creative Commons Attribution 3.0 Unported License. Original image at: File:4 vials of human cerebrospinal fluid.jpg - Wikimedia Commons.
Replace the stylet before removing the needle from the patient. Clean the site and apply a clean dressing. There is no convincing data to support a recommendation of bed rest after the procedure. Patients no longer have to lay flat on their back for one hour as previously recommended.
Lab studies
Inspect the fluid by holding it in front of a white piece of paper in good light.
Is it turbid, cloudy or bloody appearing? Order lab analysis as follows:
- Tube 1: Cell count and differential
- Tube 2: Gram stain, bacterial and viral cultures
- Tube 3: Glucose, protein, protein electrophoresis (if indicated)
- Tube 4: Second cell count and differential.
- Tube 3 or 4 can be used for special tests or additional cultures
CSF Interpretation
Interpretation of the CSF lab analysis requires looking at all available results together. Table 2 lists the lab analysis findings for the most common emergency room indications for lumbar puncture. All CSF analysis results should be interpreted in the context of the clinical presentation.
Table 2: CSF Interpretation | |||||
|---|---|---|---|---|---|
Diagnosis | Glucose (50-80 mg/dL) | Protein (15-45 mg/dL) | WBC (<5cells/uL) | RBC(0-500 cells/uL*) | Other |
Bacterial Meningitis | Low | Elevated, >50 | Elevated 500-10,000, PMN predominance | Normal | +Gram Stain, High opening pressure |
Viral Meningitis | Normal | Normal to slightly elevated | Elevated, 6-1000, Lymphocyte predominance | Variable | High RBCs can be seen in herpes encephalitis |
Tuberculosis | Low | High | High | Normal | |
Subarachnoid Hemorrhage | Normal | Normal | Normal | High +xantho-chromia | If tube 4 is less than 500 cells/uL most likely traumatic* |
Guillain Barre Syndrome | Normal | High | Normal | Normal | |
Multiple Sclerosis | Normal | Normal | Normal | Normal | Oligoclonal bands on electrophoresis |
The normal number of RBCs in CSF is zero, but traumatic taps are common due to the epidural vascular plexus. There is no clear consensus on “how low is acceptable” when evaluating for SAH. The number of RBCs should decrease from Tube 1 to Tube 4. Correlation with clinical suspicion is often needed, and the lumbar puncture may need to be repeated.
Complications of lumbar puncture
1. Post-lumbar puncture headache is the most common complication (10-30%). It results from lower CSF pressure or continued CSF leak.
Treatment
- Headaches usually respond well to analgesics and IV caffeine therapy. In more severe cases, an epidural blood patch may be required for definitive management.
- Of note, it is no longer recommended to have patients lie flat on their back for one hour as data studies found it does not prevent headache.
2. Epidural or subdural hematoma develop hours to days after the procedure. Patients will typically present with severe low back pain and may have neurological symptoms suggestive of cord compression and cauda equina. A prompt MRI should be performed.
Treatment
- Symptomatic patients likely will require surgical intervention to prevent permanent neurological deficits.
3. Iatrogenic infections are reduced by proper sterile technique. Still, inadvertent introduction of bacteria during the procedure may result in a spinal abscess, discitis, or meningitis. Typically these infections take weeks to develop.
Treatment
- Large abscesses may require surgical intervention. Discitis and meningitis may require prolonged courses of antibiotics.
4. Cerebral herniation is the most feared complication. If a patient develops rapid neurologic deterioration following lumbar puncture, reimage the patient immediately
Treatment
- Elevate head of the bed, consider hypertonic saline or mannitol and promptly consult neurosurgery for emergent management.
- See “special considerations” below to understand which populations are at higher risk for herniation.
5. Epidermoid tumors rarely occur as a complication from prior lumbar puncture and are more commonly congenital lesions. Risk can be mitigated by the use of the stylet, as to avoid introduction of skin into the spinal canal. Epidermoid tumors occur more commonly in pediatric patients and may take years to develop
Treatment
- May involve radiation, chemotherapy, and or surgical excision.
Special considerations
Generally, a lumbar puncture can be performed without a prior head CT in neurologically intact patients. A CT scan should be done prior to lumbar puncture if there is concern for mass or brain edema as this might increase the chance of herniation following CSF removal. There are a few patient populations that warrant a CT head prior to a lumbar puncture. This includes immunocompromised patients such as patients with HIV, and patients with a focal neurological deficit, depressed mental status or with papilledema. A CT does not rule out the possibility of increased intracranial pressure.
If suspicion for CNS infection is high, do not let performance of an lumbar puncture delay the administration of appropriate empiric antibiotics. Pretreatment with antibiotics might decrease the yield of fluid cultures. Delaying treatment in severely ill patients will be detrimental to their outcome!
Pearls and Pitfalls
Proper initial set-up and positioning for the procedure are the most critical steps and will help you safely and successfully perform a lumbar puncture.
Position yourself properly - raise the bed so that it’s comfortable for you
Position the patient properly - have someone to help coach or hold the patient in a position with the back arched to open the spinous processes
Position supplies in the room properly - position your stand with supplies close enough to reach without having to turn around. Bring a garbage can close to throw away packaging.
Do not delay antibiotic administration to obtain the lumbar puncture
Patients do not need to lay flat after lumbar puncture, as recent studies suggest it shows no benefit in reducing incidence of post lumbar puncture headache.
Prior to entering the skin with the needle make sure you set-up the manometer and CSF collection tubes (place in order from #1 to #4 with caps off).
- LOAD THE BOAT - Have another team member in the room with you. Ask for help if you need it, and ask for it earlier rather than later.
Case Study Resolution
The patient was found to have a leukocytosis to 20.5 with neutrophil predominance. CT head was negative for intracranial pathology. After she was intubated in the emergency department, the excellent medical student performed a diagnostic lumbar puncture. She was started on empiric antibiotics and transferred to the medical intensive care unit. On hospital day 2, her CSF studies revealed gram positive cocci in chains. Her blood cultures grew streptococcus pneumoniae, and her antibiotics were narrowed to ceftriaxone and vancomycin. On hospital day 4, her mental status improved and she was successfully extubated and transferred to the floor. She was discharged on hospital day 6 with her son.
References
Euerle B. 2013 Spinal Puncture and Cerebrospinal Fluid Examination (60). In Roberts and Hedges’ Clinical Procedures in Emergency Medicine.
Reichman E. 2004 Lumbar Puncture (96). In Emergency Medicine Procedures.
Silver B. Lumbar puncture. N Engl J Med. 2007 Jan 25;356(4):424-5
N Engl J Med 2004; 351:1849-1859; DOI: 10.1056/NEJMoa040845 http://www.nejm.org/doi/full/10.1056/NEJMvcm054952 NEJM Videos.
Lumbar Puncture (n.d) In UCSF Procedures Training. Retrieved from http://sfgh.medicine.ucsf.edu/education/resed/procedures/lumbarpuncture/
Doherty CM, Forbes RB. Diagnostic lumbar puncture. Ulster Med J. 2014 May;83(2):93-102.
Perry JJ, Stiell IG, Sivilotti ML, Bullard MJ, Emond M, Symington C, Sutherland J, Worster A, Hohl C, Lee JS, Eisenhauer MA, Mortensen M, Mackey D, Pauls M, Lesiuk H, Wells GA. Sensitivity of computed tomography performed within six hours of onset of headache for diagnosis of subarachnoid haemorrhage: prospective cohort study. BMJ. 2011 Jul 18;343:d4277. doi: 10.1136/bmj.d4277. PMID: 21768192; PMCID: PMC3138338.
Thompson AJ, Banwell BL, Barkhof F, Carroll WM, Coetzee T, Comi G, Correale J, Fazekas F, Filippi M, Freedman MS, Fujihara K, Galetta SL, Hartung HP, Kappos L, Lublin FD, Marrie RA, Miller AE, Miller DH, Montalban X, Mowry EM, Sorensen PS, Tintoré M, Traboulsee AL, Trojano M, Uitdehaag BMJ, Vukusic S, Waubant E, Weinshenker BG, Reingold SC, Cohen JA. Diagnosis of multiple sclerosis: 2017 revisions of the McDonald criteria. Lancet Neurol. 2018 Feb;17(2):162-173. doi: 10.1016/S1474-4422(17)30470-2. Epub 2017 Dec 21. PMID: 29275977.
Bodilsen J, Dalager-Pedersen M, Schønheyder HC, Nielsen H. Time to antibiotic therapy and outcome in bacterial meningitis: a Danish population-based cohort study. BMC Infect Dis. 2016 Aug 9;16:392. doi: 10.1186/s12879-016-1711-z. PMID: 27507415; PMCID: PMC4977612.
Lin A, Foroozan R, Danesh-Meyer HV, De Salvo G, Savino PJ, Sergott RC. Occurrence of cerebral venous sinus thrombosis in patients with presumed idiopathic intracranial hypertension. Ophthalmology. 2006 Dec;113(12):2281-4. doi: 10.1016/j.ophtha.2006.05.065. PMID: 17157135.
Rudnick E, Sismanis A. Pulsatile tinnitus and spontaneous cerebrospinal fluid rhinorrhea: indicators of benign intracranial hypertension syndrome. Otol Neurotol. 2005 Mar;26(2):166-8. doi: 10.1097/00129492-200503000-00006. PMID: 15793399.
Monserrate AE, Ryman DC, Ma S, Xiong C, Noble JM, Ringman JM, Morris JC, Danek A, Müller-Sarnowski F, Clifford DB, McDade EM, Brooks WS, Darby DG, Masters CL, Weston PS, Farlow MR, Graff-Radford NR, Salloway SP, Fagan AM, Oliver A, Bateman RJ; Dominantly Inherited Alzheimer Network. Factors associated with the onset and persistence of post-lumbar puncture headache. JAMA Neurol. 2015 Mar;72(3):325-32. doi: 10.1001/jamaneurol.2014.3974. PMID: 25622095; PMCID: PMC4364538.
Boonmak P, Boonmak S. Epidural blood patching for preventing and treating post-dural puncture headache. Cochrane Database Syst Rev. 2010 Jan 20;(1):CD001791. doi: 10.1002/14651858.CD001791.pub2. Update in: Cochrane Database Syst Rev. 2013;11:CD001791. PMID: 20091522.
Wall M, Kupersmith MJ, Kieburtz KD, Corbett JJ, Feldon SE, Friedman DI, Katz DM, Keltner JL, Schron EB, McDermott MP; NORDIC Idiopathic Intracranial Hypertension Study Group. The idiopathic intracranial hypertension treatment trial: clinical profile at baseline. JAMA Neurol. 2014 Jun;71(6):693-701. doi: 10.1001/jamaneurol.2014.133. PMID: 24756302; PMCID: PMC4351808.
Arevalo-Rodriguez I, Ciapponi A, Roqué i Figuls M, Muñoz L, Bonfill Cosp X. Posture and fluids for preventing post-dural puncture headache. Cochrane Database Syst Rev. 2016 Mar 7;3(3):CD009199. doi: 10.1002/14651858.CD009199.pub3. PMID: 26950232; PMCID: PMC6682345.
Bhatoe HS, Gill HS, Kumar N, Biswas S. Post lumbar puncture discitis and vertebral collapse. Postgrad Med J. 1994 Dec;70(830):882-4. doi: 10.1136/pgmj.70.830.882. PMID: 7870634; PMCID: PMC2398020.
Issaivanan M, Cohen S, Mittler M, Johnson A, Edelman M, Redner A. Iatrogenic spinal epidermoid cyst after lumbar puncture using needles with stylet. Pediatr Hematol Oncol. 2011 Oct;28(7):600-3. doi: 10.3109/08880018.2011.613093. PMID: 21936622.
